Comprehensive and Detailed Explanation From Exact Extract (NCC C-EFM sources: AWHONN, Miller’s Pocket Guide, Menihan, Simpson, Creasy & Resnik, 2025 Candidate Guide)
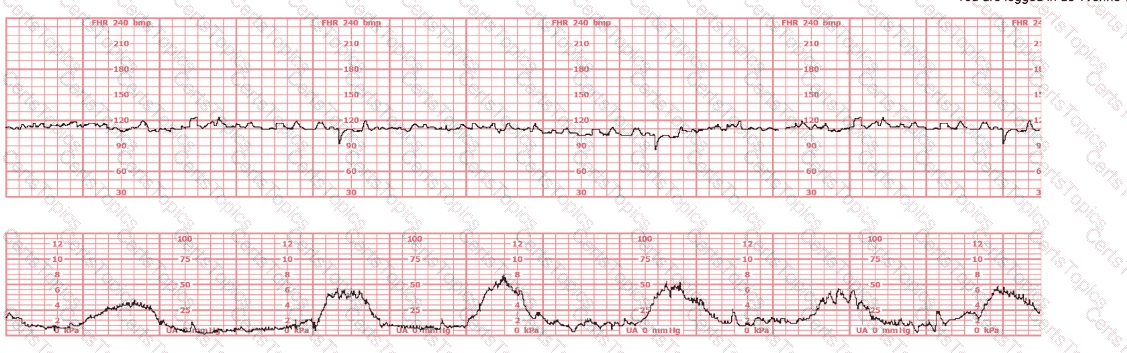
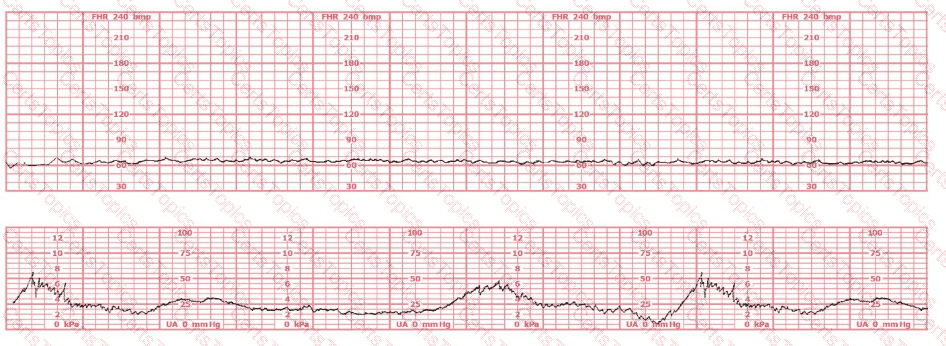
The tracing displays baseline fetal bradycardia, with a rate near 100 bpm, minimal variability, and preserved periodic response. According to AWHONN’s Fetal Heart Monitoring Principles & Practices and Menihan’s Electronic Fetal Monitoring, maternal conditions that reduce oxygen-carrying capacity—including maternal anemia—can lead to lower fetal oxygen delivery, prompting a fetal compensatory bradycardic baseline.
Creasy & Resnik’s Maternal-Fetal Medicine notes that sickle cell anemia decreases maternal hemoglobin function even when maternal vital signs appear stable, reducing uteroplacental oxygen transport. Fetuses of mothers with sickling disorders may demonstrate lower resting fetal heart rates due to chronic mild hypoxemia.
Conversely, Eisenmenger’s syndrome is associated with severe maternal cyanosis and high fetal mortality, often producing late decelerations and growth restriction rather than mild bradycardia. Systemic lupus erythematosus (SLE) is commonly associated with heart block (especially with anti-Ro/SSA antibodies), which is not displayed here, as true heart block presents with a fixed atrial–ventricular dissociation and FHR < 60 bpm.
Thus, based on fetal physiology and maternal disease correlations taught in NCC-recommended sources, the tracing is most consistent with maternal sickle cell anemia.