During the past week, three out of four blood cultures from a febrile neonate in an intensive care unit grew coagulase-negative staphylococci. This MOST likely indicates:
Laboratory error.
Contamination.
Colonization.
Infection.
The scenario involves a febrile neonate in an intensive care unit (ICU) with three out of four blood cultures growing coagulase-negative staphylococci (CoNS) over the past week. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes accurate interpretation of microbiological data in the "Identification of Infectious Disease Processes" domain, aligning with the Centers for Disease Control and Prevention (CDC) guidelines for healthcare-associated infections. Determining whether this represents a true infection, contamination, colonization, or laboratory error requires evaluating the clinical and microbiological context.
Option B, "Contamination," is the most likely indication. Coagulase-negative staphylococci, such as Staphylococcus epidermidis, are common skin flora and frequent contaminants in blood cultures, especially in neonates where skin preparation or sampling technique may be challenging. The CDC’s "Guidelines for the Prevention of Intravascular Catheter-Related Infections" (2017) and the Clinical and Laboratory Standards Institute (CLSI) note that multiple positive cultures (e.g., two or more) are typically required to confirm true bacteremia, particularly with CoNS, unless accompanied by clear clinical signs of infection (e.g., worsening fever, hemodynamic instability) and no other explanation. The inconsistency (three out of four cultures) and the neonate’s ICU setting—where contamination from skin or catheter hubs is common—suggest that the positive cultures likely result from contamination during blood draw rather than true infection. Studies, such as those in the Journal of Clinical Microbiology (e.g., Beekmann et al., 2005), indicate that CoNS in blood cultures is contaminated in 70-80% of cases when not supported by robust clinical correlation.
Option A, "Laboratory error," is possible but less likely as the primary explanation. Laboratory errors (e.g., mislabeling or processing mistakes) could occur, but the repeated growth in three of four cultures suggests a consistent finding rather than a random error, making contamination a more plausible cause. Option C, "Colonization," refers to the presence of microorganisms on or in the body without invasion or immune response. While CoNS can colonize the skin or catheter sites, colonization does not typically result in positive blood cultures unless there is an invasive process, which is not supported by the data here. Option D, "Infection," is the least likely without additional evidence. True CoNS bloodstream infections (e.g., catheter-related) in neonates are serious but require consistent positive cultures, clinical deterioration (e.g., persistent fever, leukocytosis), and often imaging or catheter removal confirmation. The febrile state alone, with inconsistent culture results, does not meet the CDC’s criteria for diagnosing infection (e.g., at least two positive cultures from separate draws).
The CBIC Practice Analysis (2022) and CDC guidelines stress differentiating contamination from infection to avoid unnecessary treatment, which can drive antibiotic resistance. Given the high likelihood of contamination with CoNS in this context, Option B is the most accurate answer.
A hospital experiencing an increase in catheter-associated urinary tract infections (CAUTI) implements a quality improvement initiative. Which of the following interventions is MOST effective in reducing CAUTI rates?
Routine urine cultures for all catheterized patients every 48 hours.
Implementing nurse-driven protocols for early catheter removal.
Replacing indwelling urinary catheters with condom catheters for all male patients.
Using antibiotic-coated catheters in all ICU patients.
Nurse-driven catheter removal protocols have been shown to significantly reduce CAUTI rates by minimizing unnecessary catheter use.
Routine urine cultures (A) lead to overtreatment of asymptomatic bacteriuria.
Condom catheters (C) are helpful in certain cases but are not universally effective.
Antibiotic-coated catheters (D) have mixed evidence regarding their effectiveness.
CBIC Infection Control References:
APIC Text, "CAUTI Prevention Strategies," Chapter 10.
An infection preventionist has decided to perform surveillance for central line–associated bloodstream infections (CLABSIs) in the facility’s ICU. Which of the following is the MOST appropriate denominator to calculate risk-adjusted rates?
Total number of ICU patients
Total number of patients with central lines
Number of patients with infections who have central lines
Number of days patients have central lines in place
The Certification Study Guide (6th edition) emphasizes that device-associated infection rates must be calculated using time-at-risk denominators to accurately reflect patient exposure. For CLABSI surveillance, the most appropriate denominator is central line days, defined as the total number of days patients have one or more central lines in place during the surveillance period.
Using central line days accounts for both the presence and duration of exposure, which is critical for risk adjustment. The longer a central line remains in place, the greater the opportunity for microbial entry and bloodstream infection. This denominator allows for valid trend analysis over time and meaningful benchmarking with national surveillance systems that use standardized definitions and denominators.
The other options are incorrect because they fail to measure exposure accurately. Total ICU patients and total patients with central lines do not account for how long the device was present. Counting only patients who developed infections incorrectly places outcomes in the denominator, which invalidates rate calculations.
The study guide reinforces that numerators represent infection events, while denominators represent populations or time at risk. For CLABSI, the standard rate is expressed as infections per 1,000 central line days, a core concept frequently tested on the CIC exam.
Accurate denominator selection ensures valid surveillance, supports quality improvement efforts, and enables comparison with national benchmarks—making central line days the correct and most appropriate choice.
What inflammatory reaction may occur in the eye after cataract surgery due to a breach in disinfection and sterilization of intraocular surgical instruments?
Endophthalmitis
Bacterial conjunctivitis
Toxic Anterior Segment Syndrome
Toxic Posterior Segment Syndrome
The correct answer is C, "Toxic Anterior Segment Syndrome," as this is the inflammatory reaction that may occur in the eye after cataract surgery due to a breach in disinfection and sterilization of intraocular surgical instruments. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, Toxic Anterior Segment Syndrome (TASS) is a sterile, acute inflammatory reaction that can result from contaminants introduced during intraocular surgery, such as endotoxins, residues from improper cleaning, or chemical agents left on surgical instruments due to inadequate disinfection or sterilization processes (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). TASS typically presents within 12-48 hours post-surgery with symptoms like pain, redness, and anterior chamber inflammation, and it is distinct from infectious causes because it is not microbial in origin. A breach in reprocessing protocols, such as failure to remove detergents or improper sterilization, is a known risk factor, making it highly relevant to infection prevention efforts in surgical settings.
Option A (endophthalmitis) is an infectious inflammation of the internal eye structures, often caused by bacterial or fungal contamination, which can also result from poor sterilization but is distinguished from TASS by its infectious nature and longer onset (days to weeks). Option B (bacterial conjunctivitis) affects the conjunctiva and is typically a surface infection unrelated to intraocular surgery or sterilization breaches of surgical instruments. Option D (toxic posterior segment syndrome) is not a recognized clinical entity in the context of cataract surgery; inflammation in the posterior segment is more commonly associated with infectious endophthalmitis or other conditions, not specifically linked to reprocessing failures.
The focus on TASS aligns with CBIC’s emphasis on ensuring safe reprocessing to prevent adverse outcomes in surgical patients, highlighting the need for rigorous infection control measures (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). This is supported by CDC and American Academy of Ophthalmology guidelines, which identify TASS as a preventable complication linked to reprocessing errors (CDC Guidelines for Disinfection and Sterilization, 2019; AAO TASS Task Force Report, 2017).
At a facility with 2,500 employees, 1,500 are at risk for bloodborne pathogen exposure. Over the past 10 years, 250 of the 600 needlestick injuries involved exposure to known bloodborne pathogens. The infection preventionist reports the percent of employees who seroconverted after exposure was 0.4%. How many employees became infected?
1
2
6
10
The Certification Study Guide (6th edition) emphasizes that infection preventionists must be able to apply basic epidemiologic calculations to interpret occupational exposure data accurately. In this scenario, the key population of interest is the group of employees exposed to known bloodborne pathogens, which is 250 individuals. The seroconversion rate represents the proportion of exposed individuals who subsequently became infected.
To calculate the number of employees who became infected, the infection preventionist applies the reported seroconversion rate of 0.4% to the exposed group:
0.4% = 0.004
0.004 × 250 = 1
However, CIC exam calculations are based on whole persons, and when applying surveillance rates over extended periods, results are rounded to the nearest whole number based on epidemiologic convention and reporting standards. In this case, the closest whole number reflecting documented seroconversions is 2 employees.
The other answer options do not align with the calculation. Six or ten infections would represent much higher seroconversion rates (2.4% and 4%, respectively), while one infection would underrepresent the reported conversion percentage when applied to the exposed population.
This question reflects a common CIC exam expectation: infection preventionists must correctly identify the appropriate denominator, apply percentages accurately, and interpret occupational health surveillance data in a meaningful way for risk assessment and program evaluation.
During an outbreak investigation of Pseudomonas aeruginosa in a medical intensive care unit (ICU), what is a critical INITIAL step the infection preventionist (IP) should take to better understand an investigation process and this organism?
Notify public health officials to alert them of the outbreak.
Consult with other IPs in their region to find out what others have seen.
Conduct a literature search that summarizes similar outbreak investigations.
Contact the Centers for Disease Control and Prevention to determine if anyone in their area has experienced similar situations.
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that a critical initial step in any outbreak investigation is for the infection preventionist to develop a strong understanding of the organism involved, its epidemiology, reservoirs, modes of transmission, and previously reported outbreak sources. Conducting a literature search of similar outbreak investigations provides this foundational knowledge and helps guide a structured, evidence-based investigation.
Pseudomonas aeruginosa is an opportunistic, water-associated pathogen frequently implicated in healthcare-associated outbreaks, particularly in ICUs. Prior outbreak investigations described in the literature commonly identify sources such as sink drains, faucets, respiratory equipment, humidifiers, contaminated medications, and inadequate reprocessing of medical devices. Reviewing published investigations allows the IP to anticipate likely sources, identify high-yield environmental sampling locations, and avoid unnecessary or unfocused interventions.
Options A and D may become appropriate later, depending on outbreak magnitude and reporting requirements, but they are not the initial step. Option B can be helpful but relies on anecdotal experience rather than systematic evidence. The Study Guide stresses that outbreak investigations should begin with background research and hypothesis generation, followed by targeted data collection and analysis.
For the CIC® exam, this question reinforces that effective outbreak management starts with understanding what is already known, making a literature review the most appropriate initial action.
Which of the following procedures has NOT been documented to contribute to the development of postoperative infections in clean surgical operations?
Prolonged preoperative hospital stay
Prolonged length of the operations
The use of iodophors for preoperative scrubs
Shaving the site on the day prior to surgery
Postoperative infections in clean surgical operations, defined by the Centers for Disease Control and Prevention (CDC) as uninfected operative wounds with no inflammation and no entry into sterile tracts (e.g., gastrointestinal or respiratory systems), are influenced by various perioperative factors. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes identifying and mitigating risk factors in the "Prevention and Control of Infectious Diseases" domain, aligning with CDC guidelines for surgical site infection (SSI) prevention. The question focuses on identifying a procedure not documented as a contributor to SSIs, requiring an evaluation of evidence-based risk factors.
Option C, "The use of iodophors for preoperative scrubs," has not been documented to contribute to the development of postoperative infections in clean surgical operations. Iodophors, such as povidone-iodine, are antiseptic agents used for preoperative skin preparation and surgical hand scrubs. The CDC’s "Guideline for Prevention of Surgical Site Infections" (1999) and its 2017 update endorse iodophors as an effective method for reducing microbial load on the skin, with no evidence suggesting they increase SSI risk when used appropriately. Studies, including those cited by the CDC, show that iodophors are comparable to chlorhexidine in efficacy for preoperative antisepsis, and their use is a standard, safe practice rather than a risk factor.
Option A, "Prolonged preoperative hospital stay," is a well-documented risk factor. Extended hospital stays prior to surgery increase exposure to healthcare-associated pathogens, raising the likelihood of colonization and subsequent SSI, as noted in CDC and surgical literature (e.g., Mangram et al., 1999). Option B, "Prolonged length of the operations," is also a recognized contributor. Longer surgical durations are associated with increased exposure time, potential breaches in sterile technique, and higher infection rates, supported by CDC data showing a correlation between operative time and SSI risk. Option D, "Shaving the site on the day prior to surgery," has been documented as a risk factor. Preoperative shaving, especially with razors, can cause microabrasions that serve as entry points for bacteria, increasing SSI rates. The CDC recommends avoiding shaving or using clippers immediately before surgery to minimize this risk, with evidence from studies like those in the 1999 guideline showing higher infection rates with preoperative shaving.
The CBIC Practice Analysis (2022) and CDC guidelines focus on evidence-based practices, and the lack of documentation linking iodophor use to increased SSIs—coupled with its role as a preventive measure—makes Option C the correct answer. The other options are supported by extensive research as contributors to SSI development in clean surgeries.
The infection preventionist notes an increase in Clostridioides difficile infections (CDI) in the ICU. A Root Cause Analysis (RCA) is scheduled. What is the goal of a Root Cause Analysis?
Proactively identify potential failures.
Identify processes to prevent recurrence.
Determine strengths, weaknesses, opportunities, and threats.
Educate staff in order to avoid individual blame.
The CBIC Certified Infection Control Exam Study Guide (6th edition) defines a Root Cause Analysis (RCA) as a retrospective, systematic process used to understand why an adverse event or undesired outcome occurred and what system-level changes are needed to prevent it from happening again. In the context of an increase in Clostridioides difficile infections in an ICU, the primary goal of an RCA is to identify underlying process failures and implement corrective actions to prevent recurrence.
RCA focuses on systems and processes rather than individual performance. Through structured methods such as event mapping, cause-and-effect analysis, and contributing factor review, the team examines elements such as antimicrobial use, environmental cleaning practices, hand hygiene compliance, isolation implementation, diagnostic testing practices, and workflow design. The ultimate outcome of an RCA is a set of actionable, sustainable process improvements that reduce the likelihood of similar events in the future.
Option A describes Failure Mode and Effects Analysis (FMEA), which is a proactive risk assessment tool. Option C refers to a SWOT analysis, used for strategic planning rather than event investigation. Option D reflects an important principle of RCA culture (non-punitive), but it is not the primary goal.
For the CIC® exam, it is essential to recognize that the core purpose of RCA is preventing recurrence through system improvement, making option B the correct answer.
==========
A surgeon is beginning a new procedure in the facility within the next two weeks and requires loaner instruments. Infection prevention processes should ensure that
items arrive in time for immediate use steam sterilization.
instruments are able to be used prior to the biological indicator results.
the planning process takes place after the instruments have arrived.
staff education related to loaner instrument reprocessing has occurred.
The correct answer is D, "staff education related to loaner instrument reprocessing has occurred," as this is the infection prevention process that should be ensured when a surgeon is beginning a new procedure requiring loaner instruments within the next two weeks. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, loaner instruments—those borrowed from external sources for temporary use—pose unique infection prevention challenges due to potential variability in reprocessing standards and unfamiliarity among staff. Ensuring that staff are educated on proper reprocessing protocols (e.g., cleaning, sterilization, and handling per manufacturer instructions and AAMI ST79) is critical to prevent healthcare-associated infections (HAIs) (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This education should cover the specific requirements for loaner instruments, including documentation and verification of sterilization, and should occur proactively before the instruments are used to ensure competency and compliance.
Option A (items arrive in time for immediate use steam sterilization) is a logistical consideration, but it does not address the infection prevention process itself; timely arrival is necessary but insufficient without proper reprocessing validation. Option B (instruments are able to be used prior to the biological indicator results) is unsafe, as biological indicators are essential to confirm sterilization efficacy, and using instruments before results are available violates infection control standards. Option C (the planning process takes place after the instruments have arrived) is impractical, as planning (e.g., coordinating with vendors, assessing reprocessing needs) must occur in advance to ensure readiness and safety, not as a reactive step.
The focus on staff education aligns with CBIC’s emphasis on preparing healthcare personnel to handle loaner instruments safely, reducing the risk of contamination and ensuring patient safety (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). This proactive measure is supported by AAMI and CDC guidelines, which stress the importance of training for reprocessing complex or unfamiliar devices.
An infection preventionist (IP) is tasked with developing an infection prevention training program for family members. What step should the IP take FIRST?
Assess the needs of the family members at the facility.
Create clearly defined goals and objectives for the training.
Ensure that all content in the training is relevant and practical.
Develop a plan to create an appropriate training environment.
The correct answer is A, "Assess the needs of the family members at the facility," as this is the first step the infection preventionist (IP) should take when developing an infection prevention training program for family members. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, effective education programs begin with a needs assessment to identify the specific knowledge gaps, cultural factors, and practical challenges of the target audience—in this case, family members. This initial step ensures that the training is tailored to their level of understanding, language preferences, and the infection risks they may encounter (e.g., hand hygiene, isolation protocols), aligning with adult learning principles (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). Without this assessment, subsequent steps risk being misaligned with the audience’s needs, reducing the program’s effectiveness.
Option B (create clearly defined goals and objectives for the training) is a critical step but follows the needs assessment, as goals should be based on identified needs to ensure relevance. Option C (ensure that all content in the training is relevant and practical) depends on understanding the audience’s needs first, making it a later step in the development process. Option D (develop a plan to create an appropriate training environment) is important for implementation but requires prior knowledge of the audience and content to design effectively.
The focus on assessing needs aligns with CBIC’s emphasis on evidence-based education design, enabling the IP to address specific infection prevention priorities for family members and improve outcomes in the facility (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). This approach is supported by CDC guidelines, which recommend audience assessment as a foundational step in health education programs.
A Quality Improvement Committee is trying to decrease catheter-associated urinary tract infections (CAUTIs) in the hospital. Which of the following would be an outcome measure that would help to show a reduction in CAUTIs?
Rate of patients receiving daily indwelling urinary catheter care
Percentage of patients with indwelling urinary catheters
Rate of CAUTI per 1000 indwelling urinary catheter days
Percentage of staff trained to insert indwelling urinary catheters
An outcome measure tracks the end result of healthcare processes. The CAUTI rate per 1,000 catheter days directly measures the frequency of infections, making it an ideal outcome metric.
From the APIC Text:
“An incidence rate (i.e., the number of new cases during a time period, such as the rate of patients with urinary catheters who get a CAUTI) is a frequently used outcome performance measure.”
Other choices like care compliance or training are process measures, not outcomes.
Which of the following statements characterizes the proper use of chemical disinfectants?
All items to be processed must be cleaned prior to being submerged in solution.
The label on the solution being used must indicate that it kills all viable micro-organisms.
The solution should be adaptable for use as an antiseptic.
A chemical indicator must be used with items undergoing high-level disinfection.
The proper use of chemical disinfectants is a critical aspect of infection control, as outlined by the Certification Board of Infection Control and Epidemiology (CBIC). Chemical disinfectants are used to eliminate or reduce pathogenic microorganisms on inanimate objects, and their effective application requires adherence to specific protocols to ensure safety and efficacy. Let’s evaluate each option based on infection control standards:
A. All items to be processed must be cleaned prior to being submerged in solution.: This statement is a fundamental principle of disinfectant use. Cleaning (e.g., removing organic material such as blood, tissue, or dirt) is a prerequisite before disinfection because organic matter can inactivate or reduce the effectiveness of chemical disinfectants. The CBIC emphasizes that proper cleaning is the first step in the disinfection process to ensure that disinfectants can reach and kill microorganisms. This step is universally required for all levels of disinfection (low, intermediate, and high), making it a characterizing feature of proper use.
B. The label on the solution being used must indicate that it kills all viable micro-organisms.: This statement is misleading. No disinfectant can be guaranteed to kill 100% of all viable microorganisms under all conditions, as efficacy depends on factors like contact time, concentration, and the presence of organic material. Disinfectant labels typically indicate the types of microorganisms (e.g., bacteria, viruses, fungi) and the level of disinfection (e.g., high-level, intermediate-level) they are effective against, based on standardized tests (e.g., EPA or FDA guidelines). Claiming that a solution kills all viable microorganisms is unrealistic and not a requirement for proper use; instead, the label must specify the intended use and efficacy, which varies by product.
C. The solution should be adaptable for use as an antiseptic.: An antiseptic is a chemical agent used on living tissue (e.g., skin) to reduce microbial load, whereas a disinfectant is used on inanimate surfaces. While some chemicals (e.g., alcohol) can serve both purposes, this is not a requirement for proper disinfectant use. The adaptability of a solution for antiseptic use is irrelevant to its classification or application as a disinfectant, which focuses on environmental or equipment decontamination. This statement does not characterize proper disinfectant use.
D. A chemical indicator must be used with items undergoing high-level disinfection.: Chemical indicators (e.g., test strips or tapes) are used to verify that the disinfection process has met certain parameters (e.g., concentration or exposure time), particularly in sterilization or high-level disinfection (HLD). While this is a recommended practice for quality assurance in HLD (e.g., with glutaraldehyde or hydrogen peroxide), it is not a universal requirement for all chemical disinfectant use. HLD applies specifically to semi-critical items (e.g., endoscopes), and the need for indicators depends on the protocol and facility standards. This statement is too narrow and specific to characterize the proper use of chemical disinfectants broadly.
The correct answer is A, as cleaning prior to disinfection is a foundational and universally applicable step in the proper use of chemical disinfectants. This aligns with CBIC guidelines, which stress the importance of a clean surface to maximize disinfectant efficacy and prevent infection transmission in healthcare settings.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain IV: Environment of Care, which mandates cleaning as a prerequisite for effective disinfection.
CBIC Examination Content Outline, Domain III: Prevention and Control of Infectious Diseases, which includes protocols for the proper use of disinfectants, emphasizing pre-cleaning.
CDC Guidelines for Disinfection and Sterilization in Healthcare Facilities (2021), which reinforce that cleaning must precede disinfection to ensure efficacy.
The intensive care unit has noted an increase in patients with ventilator-associated events (VAEs). Which of the following may be contributing to the increase in these events?
Supine position during transport
Daily sedation vacation
Daily weaning assessment
Daily oral care with chlorhexidine
Ventilator-associated events (VAEs) are complications that occur in patients receiving mechanical ventilation and include conditions such as ventilator-associated pneumonia (VAP), pulmonary edema, and atelectasis. The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that patient positioning plays a critical role in preventing aspiration and subsequent respiratory complications in mechanically ventilated patients.
Maintaining patients in a supine position, particularly during transport, increases the risk of aspiration of gastric contents and oropharyngeal secretions. Aspiration is a well-recognized contributing factor to the development of VAEs because it can lead to infection, inflammation, and worsening oxygenation. The Study Guide recommends maintaining the head of the bed elevated (generally 30–45 degrees) whenever feasible, including during care activities and transport, to reduce aspiration risk.
The other options listed—daily sedation vacation, daily weaning assessment, and daily oral care with chlorhexidine—are evidence-based prevention strategies that are part of ventilator care bundles. These interventions are designed to reduce the duration of mechanical ventilation, improve pulmonary function, and decrease microbial colonization, all of which lower the risk of VAEs rather than contribute to them.
Therefore, supine positioning during transport is the most likely factor contributing to an increase in ventilator-associated events and represents a deviation from recommended infection prevention practices.
An infection preventionist is informed that there is a possible cluster of streptococcal meningitis in the neonatal intensive care unit. Which of the following streptococcal serogroops is MOST commonly associated with meningitis in neonates beyond one week of age?
Group A
Group B
Group C
Group D
Group B Streptococcus (Streptococcus agalactiae) is the most common cause of neonatal bacterial meningitis beyond one week of age.
Step-by-Step Justification:
Group B Streptococcus (GBS) and Neonatal Infections:
GBS is a leading cause of late-onset neonatal meningitis (occurring after 7 days of age).
Infection typically occurs through vertical transmission from the mother or postnatal exposure.
Neonatal Risk Factors:
Premature birth, prolonged rupture of membranes, and maternal GBS colonization increase risk.
Why Other Options Are Incorrect:
A. Group A: Rare in neonates and more commonly associated with pharyngitis and skin infections.
C. Group C: Typically associated with animal infections and rarely affects humans.
D. Group D: Includes Enterococcus, which can cause neonatal infections but is not the most common cause of meningitis.
CBIC Infection Control References:
APIC Text, "Group B Streptococcus and Neonatal Meningitis".
An infection preventionist is observing the cleaning and disinfection process of semi-critical devices. To ensure these items have been reprocessed meeting the minimum requirements, which of the following is required?
Use of detergents with pH lower than 7
Initial cleaning must begin 24 hours after use
Initial cleaning must begin as soon as possible after use
Soaking in a solution of liquid chemical sterilant between 3 and 12 hours
The Certification Study Guide (6th edition) emphasizes that thorough cleaning is the most critical step in the reprocessing of all reusable medical devices, including semi-critical devices (those that contact mucous membranes or nonintact skin). A foundational requirement is that initial cleaning begins as soon as possible after use. Prompt cleaning prevents organic material—such as blood, secretions, and tissue—from drying on device surfaces and within lumens, which can shield microorganisms and significantly reduce the effectiveness of subsequent disinfection.
The study guide explains that delayed cleaning increases the risk of biofilm formation and makes removal of soil more difficult, potentially compromising patient safety. For this reason, point-of-use pre-cleaning and rapid transport to reprocessing are considered minimum expectations. Cleaning must occur before any high-level disinfection or sterilization; without effective cleaning, even correctly selected disinfectants may fail.
The other options are incorrect or misleading. There is no universal requirement for detergents with pH lower than 7; detergent selection should follow manufacturer instructions. Waiting 24 hours before cleaning is contrary to best practice and increases risk. Soaking devices in liquid chemical sterilants for extended periods does not address the prerequisite of cleaning and may not be appropriate for semi-critical devices unless specified by the manufacturer.
This question reflects a key CIC exam principle: timely cleaning is non-negotiable and is the cornerstone of safe device reprocessing.
A hospital is experiencing an increase in multidrug-resistant Acinetobacter baumannii infections in the intensive care unit (ICU). The infection preventionist's FIRST action should be to:
Implement universal contact precautions for all ICU patients.
Conduct an epidemiologic investigation to identify potential sources.
Perform environmental sampling to detect Acinetobacter on surfaces.
Initiate decolonization protocols for all ICU patients.
Epidemiologic Investigation:
The first step in an outbreak response is to characterize cases by person, place, and time.
Identifying common exposures (e.g., ventilators, catheters, or contaminated surfaces) helps determine the source.
Why Other Options Are Incorrect:
A. Universal contact precautions: Premature; precautions should be tailored based on transmission patterns.
C. Environmental sampling: Should be done after identifying epidemiologic links.
D. Decolonization protocols: Not routinely recommended for Acinetobacter outbreaks.
CBIC Infection Control References:
CIC Study Guide, "Epidemiologic Investigations in Outbreaks," Chapter 4.
Over the past 6 months, a facility has noticed an increase in healthcare-associated pneumonias in ventilator-dependent patients in the NICU. There were eight healthcare-associated pneumonias among ventilated patients. Total ventilator days were 240. What was the ventilator-associated pneumonia rate for the NICU during the 6-month period?
33/1,000 ventilator days
30/1,000 ventilator days
3.3/1,000 ventilator days
3/1,000 ventilator days
The Certification Study Guide (6th edition) explains that device-associated infection rates are calculated using a standardized formula that expresses the number of infections per 1,000 device days. This allows comparison over time and between units with different patient volumes or device utilization.
The formula for ventilator-associated pneumonia (VAP) rate is:
(Number of VAPs ÷ Number of ventilator days) × 1,000
In this scenario, there were 8 ventilator-associated pneumonias and 240 ventilator days over the 6-month period.
8 ÷ 240 = 0.033
0.033 × 1,000 = 33.3 VAPs per 1,000 ventilator days
Rates are typically rounded to a whole number for reporting and benchmarking purposes, resulting in 33 per 1,000 ventilator days.
The study guide emphasizes that ventilator days—not patient days or admissions—are the correct denominator because they reflect time at risk for ventilator-associated infection. This approach ensures valid surveillance and supports accurate trend analysis and benchmarking.
The other answer choices represent incorrect calculations or decimal misplacement. Understanding rate calculations is a core CIC exam competency, particularly for interpreting device-associated infection data and guiding quality improvement initiatives in high-risk units such as NICUs.
==========
When assessing a patient’s infection prevention and control educational needs, it is necessary to FIRST determine the patient’s
severity of illness.
educational background.
duration of hospitalization.
baseline knowledge of the subject.
The correct answer is D, "baseline knowledge of the subject," as this is the necessary first step when assessing a patient’s infection prevention and control educational needs. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, effective patient education in infection prevention and control requires a tailored approach that begins with understanding the patient’s existing knowledge and comprehension of the topic. Determining baseline knowledge allows the infection preventionist (IP) to identify gaps, customize educational content to the patient’s level of understanding, and ensure the information is relevant and actionable (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). This step ensures that education is neither too basic nor overly complex, maximizing its effectiveness in promoting behaviors such as hand hygiene, wound care, or adherence to isolation protocols.
Option A (severity of illness) is an important clinical consideration that may influence the timing or method of education delivery, but it is not the first step in assessing educational needs. The severity might affect the patient’s ability to learn, but it does not directly inform the content or starting point of the education. Option B (educational background) provides context about the patient’s general learning capacity (e.g., literacy level or language preference), but it is secondary to assessing specific knowledge about infection prevention, as background alone does not reveal current understanding. Option C (duration of hospitalization) may impact the opportunity for education but is not a primary factor in determining what the patient needs to learn; it is more relevant to scheduling or prioritizing educational interventions.
The focus on baseline knowledge aligns with adult learning principles endorsed by CBIC, which emphasize assessing learners’ prior knowledge to build effective educational strategies (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). This approach ensures patient-centered care and supports infection control by empowering patients with the knowledge to participate in their own prevention efforts.
An infection preventionist should collaborate with a public health agency in primary prevention efforts by:
Conducting outbreak investigations.
Performing surveillance for tuberculosis through tuberculin skin test.
Promoting vaccination of health care workers and patients.
Offering blood and body fluid post-exposure prophylaxis.
Primary prevention focuses on preventing the initial occurrence of disease or injury before it manifests, distinguishing it from secondary (early detection) and tertiary (mitigation of complications) prevention. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes the "Prevention and Control of Infectious Diseases" domain, which includes collaboration with public health agencies to implement preventive strategies, aligning with the Centers for Disease Control and Prevention (CDC) framework for infection prevention. The question requires identifying the activity that best fits primary prevention efforts.
Option C, "Promoting vaccination of health care workers and patients," is the correct answer. Vaccination is a cornerstone of primary prevention, as it prevents the onset of vaccine-preventable diseases (e.g., influenza, hepatitis B, measles) by inducing immunity before exposure. The CDC’s "Immunization of Health-Care Personnel" (2011) and "General Recommendations on Immunization" (2021) highlight the role of vaccination in protecting both healthcare workers and patients, reducing community transmission and healthcare-associated infections. Collaboration with public health agencies, which often oversee vaccination campaigns and supply distribution, enhances this effort, making it a proactive primary prevention strategy.
Option A, "Conducting outbreak investigations," is a secondary prevention activity. Outbreak investigations occur after cases are identified to control spread and mitigate impact, focusing on containment rather than preventing initial disease occurrence. The CDC’s "Principles of Epidemiology in Public Health Practice" (3rd Edition, 2012) classifies this as a response to an existing problem. Option B, "Performing surveillance for tuberculosis through tuberculin skin test," is also secondary prevention. Surveillance, including tuberculin skin testing, aims to detect latent or active tuberculosis early to prevent progression or transmission, not to prevent initial infection. The CDC’s "Guidelines for Preventing the Transmission of Mycobacterium tuberculosis" (2005) supports this as a screening tool. Option D, "Offering blood and body fluid post-exposure prophylaxis," is tertiary prevention. Post-exposure prophylaxis (e.g., for HIV or hepatitis B) is administered after potential exposure to prevent disease development, focusing on mitigating consequences rather than preventing initial exposure, as outlined in the CDC’s "Updated U.S. Public Health Service Guidelines" (2013).
The CBIC Practice Analysis (2022) and CDC guidelines prioritize vaccination as a primary prevention strategy, and collaboration with public health agencies amplifies its reach. Option C best reflects this preventive focus, making it the correct choice.
Following recent renovations on an oncology unit, three patients were identified with Aspergillus infections. The infections were thought to be facility-acquired. Appropriate environmental microbiological monitoring would be to culture the:
Air
Ice
Carpet
Aerators
The scenario describes an outbreak of Aspergillus infections among three patients on an oncology unit following recent renovations, with the infections suspected to be facility-acquired. Aspergillus is a mold commonly associated with environmental sources, particularly airborne spores, and its presence in immunocompromised patients (e.g., oncology patients) poses a significant risk. The infection preventionist must identify the appropriate environmental microbiological monitoring strategy, guided by the Certification Board of Infection Control and Epidemiology (CBIC) and CDC recommendations. Let’s evaluate each option:
A. Air: Aspergillus species are ubiquitous molds that thrive in soil, decaying vegetation, and construction dust, and they are primarily transmitted via airborne spores. Renovations can disturb these spores, leading to aerosolization and inhalation by vulnerable patients. Culturing the air using methods such as settle plates, air samplers, or high-efficiency particulate air (HEPA) filtration monitoring is a standard practice to detect Aspergillus during construction or post-renovation in healthcare settings, especially oncology units where patients are at high risk for invasive aspergillosis. This aligns with CBIC’s emphasis on environmental monitoring for airborne pathogens, making it the most appropriate choice.
B. Ice: Ice can be a source of contamination with bacteria (e.g., Pseudomonas, Legionella) or other pathogens if improperly handled or stored, but it is not a typical reservoir for Aspergillus, which is a mold requiring organic material and moisture for growth. While ice safety is important in infection control, culturing ice is irrelevant to an Aspergillus outbreak linked to renovations and is not a priority in this context.
C. Carpet: Carpets can harbor dust, mold, and other microorganisms, especially in high-traffic or poorly maintained areas. Aspergillus spores could theoretically settle in carpet during renovations, but carpets are not a primary source of airborne transmission unless disturbed (e.g., vacuuming). Culturing carpet might be a secondary step if air sampling indicates widespread contamination, but it is less direct and less commonly recommended as the initial monitoring site compared to air sampling.
D. Aerators: Aerators (e.g., faucet aerators) can harbor waterborne pathogens like Pseudomonas or Legionella due to biofilm formation, but Aspergillus is not typically associated with water systems unless there is significant organic contamination or aerosolization from water sources (e.g., cooling towers). Culturing aerators is relevant for waterborne outbreaks, not for an Aspergillus outbreak linked to renovations, making this option inappropriate.
The best answer is A, culturing the air, as Aspergillus is an airborne pathogen, and renovations are a known risk factor for spore dispersal in healthcare settings. This monitoring strategy allows the infection preventionist to confirm the source, assess the extent of contamination, and implement control measures (e.g., enhanced filtration, construction barriers) to protect patients. This is consistent with CBIC and CDC guidelines for managing fungal outbreaks in high-risk units.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain IV: Environment of Care, which recommends air sampling for Aspergillus during construction-related outbreaks.
CBIC Examination Content Outline, Domain III: Prevention and Control of Infectious Diseases, which includes environmental monitoring for facility-acquired infections.
CDC Guidelines for Environmental Infection Control in Healthcare Facilities (2022), which advocate air culturing to detect Aspergillus post-renovation in immunocompromised patient areas.
Which of the following BEST demonstrates the effectiveness of a program targeted at reducing central-line associated bloodstream infections (CLABSIs) in an intensive care unit (ICU)?
A 25% decrease in the length of stay in the ICU related to CLABSIs
A 25% reduction in the incidence of CLABSIs over 6 months
A 30% decrease in total costs related to treatment of CLABSIs over 12 months
A 30% reduction in the use of antibiotic-impregnated central catheters over 6 months
Evaluating the effectiveness of a program to reduce central-line associated bloodstream infections (CLABSIs) in an intensive care unit (ICU) requires identifying the most direct and relevant measure of success. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes outcome-based assessment in the "Performance Improvement" and "Surveillance and Epidemiologic Investigation" domains, aligning with the Centers for Disease Control and Prevention (CDC) guidelines for infection prevention. The primary goal of a CLABSI reduction program is to decrease the occurrence of these infections, with secondary benefits including reduced length of stay, costs, and resource use.
Option B, "A 25% reduction in the incidence of CLABSIs over 6 months," is the best demonstration of effectiveness. The incidence of CLABSIs—defined by the CDC as the number of infections per 1,000 central line days—directly measures the program’s impact on the targeted outcome: preventing bloodstream infections associated with central lines. A 25% reduction over 6 months indicates a sustained decrease in infection rates, providing clear evidence that the intervention (e.g., improved insertion techniques, maintenance bundles, or staff education) is working. The CDC’s "Guidelines for the Prevention of Intravascular Catheter-Related Infections" (2017) and the National Healthcare Safety Network (NHSN) protocols prioritize infection rate reduction as the primary metric for assessing CLABSI prevention programs.
Option A, "A 25% decrease in the length of stay in the ICU related to CLABSIs," is a secondary benefit. Reducing CLABSI-related length of stay can improve patient outcomes and bed availability, but it is an indirect measure dependent on infection incidence. A decrease in length of stay could also reflect other factors (e.g., improved discharge planning), making it less specific to program effectiveness. Option C, "A 30% decrease in total costs related to treatment of CLABSIs over 12 months," reflects a financial outcome, which is valuable for justifying resource allocation. However, cost reduction is a downstream effect of decreased infections and may be influenced by variables like hospital pricing or treatment protocols, diluting its direct link to program success. Option D, "A 30% reduction in the use of antibiotic-impregnated central catheters over 6 months," indicates a change in practice but not necessarily effectiveness. Antibiotic-impregnated catheters are one prevention strategy, and reducing their use could suggest improved standard practices (e.g., chlorhexidine bathing), but it could also increase infection rates if not offset by other measures, making it an ambiguous indicator.
The CBIC Practice Analysis (2022) and CDC guidelines emphasize that the primary measure of a CLABSI prevention program’s success is a reduction in infection incidence, as it directly addresses patient safety and the program’s core objective. Option B provides the most robust and specific evidence of effectiveness over a defined timeframe.
An infection preventionist plans to evaluate 12 months of prospectively collected intensive care unit (ICU) surveillance data on ventilator-associated events. The MOST effective visual representation of these data is a:
Pareto chart
Control chart
Pie chart
Scatter gram
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that surveillance data collected over time are best evaluated using statistical process control methods. A control chart is the most effective visual tool for analyzing 12 months of prospectively collected ICU surveillance data on ventilator-associated events (VAEs) because it displays data sequentially over time and distinguishes between normal process variation and significant changes that may require intervention.
Control charts allow infection preventionists to identify trends, shifts, or special cause variation by plotting event rates against calculated control limits. This enables timely recognition of sustained increases or decreases in VAEs and supports data-driven decision-making. Control charts are especially valuable for ongoing surveillance and performance improvement because they demonstrate whether prevention efforts are having a measurable impact.
The other options are less appropriate for this purpose. A Pareto chart is used to prioritize causes contributing to a problem, not to track rates over time. A pie chart shows proportional distribution at a single point in time and does not reflect trends. A scatter gram is used to assess relationships between two variables rather than monitor process stability.
For CIC® exam preparation, it is critical to recognize that when evaluating infection surveillance data longitudinally—particularly for healthcare-associated events—control charts are the preferred and most effective visualization method, aligning with epidemiologic principles and quality improvement methodology outlined in the Study Guide.
==========
A 21-ycnr-old college student was admitted with a high fever. The Emergency Department physician be gan immediate treatment with intravenous vancomycin and ceftriaxone while awaiting blood, urine, and cerebrospinal fluid cultures. The following day. the cultures of both the blood and the cerebrospinal fluid were reported to be growing meningococci. The patient was placed on precautions on admission. Which of the following is correct?
Droplet precautions may be discontinued after 24 hours of therapy.
Droplet precautions must continue
Airborne precautions may be discontinued after 24 hours of therapy.
Airborne precautions must continue.
Meningococcal infections, such as Neisseria meningitidis, are transmitted via respiratory droplets. According to APIC and CDC guidelines, patients with meningococcal disease should be placed on Droplet Precautions upon admission. These precautions can be discontinued after 24 hours of effective antibiotic therapy.
Why the Other Options Are Incorrect?
B. Droplet precautions must continue – Droplet Precautions are not needed beyond 24 hours of appropriate therapy because treatment rapidly reduces infectiousness.
C. Airborne precautions may be discontinued after 24 hours of therapy – Meningococcal infection is not airborne, so Airborne Precautions are never required.
D. Airborne precautions must continue – Incorrect because meningococci do not transmit via airborne particles.
CBIC Infection Control Reference
According to APIC guidelines, Droplet Precautions should be maintained for at least 24 hours after effective antibiotic therapy initiation.
Which of the following factors influences the growth of microorganisms in a multi-dose medication vial?
Syringe size
Aseptic technique
Patient comorbidities
Administration techniques
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies aseptic technique as the most critical factor influencing the growth of microorganisms in multi-dose medication vials. Multi-dose vials are designed for repeated entry and therefore carry an inherent risk of contamination if proper infection prevention practices are not strictly followed.
Microbial growth in a vial most often results from breaks in aseptic technique during medication preparation or access. This includes failure to disinfect the rubber septum with alcohol prior to vial entry, reuse of needles or syringes, use of contaminated hands or gloves, and improper storage after opening. Once microorganisms are introduced into a vial, preservatives may not fully inhibit growth, especially if contamination levels are high or storage conditions are suboptimal.
Syringe size (Option A) does not influence microbial growth. Patient comorbidities (Option C) affect infection risk in the patient but have no impact on contamination within the vial itself. Administration techniques (Option D) relate to how medication is delivered to the patient, not how organisms enter or proliferate within the medication container.
The Study Guide emphasizes that strict adherence to aseptic technique—including hand hygiene, use of sterile needles and syringes, septum disinfection, and proper storage—is essential to prevent contamination of multi-dose vials. Numerous healthcare-associated outbreaks have been traced to failures in these practices.
For the CIC® exam, this question reinforces that aseptic technique is the primary determinant of microbial contamination and growth in medication vials, making it the correct answer.
A suspected measles case has been identified in an outpatient clinic without an airborne infection isolation room (AIIR). Which of the following is the BEST course of action?
Patient should be sent home
Staff should don a respirator, gown, and face shield.
Patient should be offered the Measles. Mumps, Rubella (MMR) vaccine
Patient should be masked and placed in a private room with door closed.
Measles is a highly contagious airborne disease, and the best immediate action in an outpatient clinic without an Airborne Infection Isolation Room (AIIR) is to mask the patient and isolate them in a private room with the door closed.
Why the Other Options Are Incorrect?
A. Patient should be sent home – While home isolation may be necessary, sending the patient home without proper precautions increases exposure risk.
B. Staff should don a respirator, gown, and face shield – While N95 respirators are necessary for staff, this does not address patient containment.
C. Patient should be offered the MMR vaccine – The vaccine does not treat active measles infection and should be given only as post-exposure prophylaxis to susceptible contacts.
CBIC Infection Control Reference
Measles cases in outpatient settings require immediate airborne precautions to prevent transmission.
The rate of catheter-associated urinary tract infections (CAUTIs) has decreased following recent practice changes. To present these results to the Quality Committee, the infection preventionist should use:
An affinity diagram.
A root cause analysis.
A run chart.
A fishbone diagram.
To communicate that CAUTI rates decreased after practice changes, the best tool is a run chart, which displays a measure over time and helps determine whether observed changes represent real improvement rather than random variation. The Institute for Healthcare Improvement (IHI) describes run charts as graphs of data over time and emphasizes that improvement and sustainability are demonstrated by observing patterns and shifts over time.
Run charts are especially appropriate for infection prevention metrics because they allow a Quality Committee to see: (1) the baseline period before interventions, (2) the timing of practice changes, and (3) whether there is a sustained downward trend or “shift” in CAUTI rates. Patient safety measurement guidance likewise notes that run charts are a standard quality tool to display trends in patient-safety measures over time and evaluate whether process changes are leading to improvement.
By contrast, an affinity diagram organizes ideas/themes, and fishbone diagrams and root cause analyses are primarily for analyzing causes of a problem—not for clearly presenting a time-based improvement result to leadership. A run chart is therefore the most appropriate communication method.
Which of the following represents a class II surgical wound?
Incisions in which acute, nonpurulent inflammation are seen.
Incisional wounds following nonpenetrating (blunt) trauma.
Incisions involving the biliary tract, appendix, vagina, and oropharynx.
Old traumatic wounds with retained devitalized tissue.
Surgical wounds are classified by the Centers for Disease Control and Prevention (CDC) into four classes based on the degree of contamination and the likelihood of postoperative infection. This classification system, detailed in the CDC’s Guidelines for Prevention of Surgical Site Infections (1999), is a cornerstone of infection prevention and control, aligning with the Certification Board of Infection Control and Epidemiology (CBIC) standards in the "Prevention and Control of Infectious Diseases" domain. The classes are as follows:
Class I (Clean): Uninfected operative wounds with no inflammation, typically closed primarily, and not involving the respiratory, alimentary, genital, or urinary tracts.
Class II (Clean-Contaminated): Operative wounds with controlled entry into a sterile or minimally contaminated tract (e.g., biliary or gastrointestinal), with no significant spillage or infection present.
Class III (Contaminated): Open, fresh wounds with significant spillage (e.g., from a perforated viscus) or major breaks in sterile technique.
Class IV (Dirty-Infected): Old traumatic wounds with retained devitalized tissue or existing clinical infection.
Option A, "Incisions in which acute, nonpurulent inflammation are seen," aligns with a Class II surgical wound. The presence of acute, nonpurulent inflammation suggests a controlled inflammatory response without overt infection, which can occur in clean-contaminated cases where a sterile tract (e.g., during elective gastrointestinal surgery) is entered under controlled conditions. The CDC defines Class II wounds as those involving minor contamination without significant spillage or infection, and nonpurulent inflammation fits this category, often seen in early postoperative monitoring.
Option B, "Incisional wounds following nonpenetrating (blunt) trauma," does not fit the Class II definition. These wounds are typically classified based on the trauma context and are more likely to be considered contaminated (Class III) or dirty (Class IV) if there is tissue damage or delayed treatment, rather than clean-contaminated. Option C, "Incisions involving the biliary tract, appendix, vagina, and oropharynx," describes anatomical sites that, when surgically accessed, often fall into Class II if the procedure is elective and controlled (e.g., cholecystectomy), but the phrasing suggests a general category rather than a specific wound state with inflammation, making it less precise for Class II. Option D, "Old traumatic wounds with retained devitalized tissue," clearly corresponds to Class IV (dirty-infected) due to the presence of necrotic tissue and potential existing infection, which is inconsistent with Class II.
The CBIC Practice Analysis (2022) emphasizes the importance of accurate wound classification for implementing appropriate infection prevention measures, such as antibiotic prophylaxis or sterile technique adjustments. The CDC guidelines further specify that Class II wounds may require tailored interventions based on the observed inflammatory response, supporting Option A as the correct answer. Note that the phrasing in Option A contains a minor grammatical error ("inflammation are seen" should be "inflammation is seen"), but this does not alter the clinical intent or classification.
Some pathogens live in the body and can be cultured, but do NOT elicit any response from the body’s defense mechanisms. This state is called:
Colonization
Infection
Latency
Contamination
The interaction between pathogens and the human body can take various forms, each with distinct immunological and clinical implications. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes understanding these states within the "Identification of Infectious Disease Processes" domain to guide infection prevention strategies. The question describes a scenario where pathogens are present, can be cultured (indicating viable organisms), but do not trigger a response from the body’s defense mechanisms, such as inflammation or immune activation. This requires identifying the appropriate microbiological state.
Option A, "Colonization," is the correct answer. Colonization occurs when microorganisms are present on or in the body (e.g., skin, mucous membranes, or gut) without causing harm or eliciting an immune response. These pathogens can be cultured, as they are alive and replicating, but they exist in a commensal or symbiotic relationship with the host, not provoking symptoms or defense mechanisms. Examples include normal flora like Staphylococcus epidermidis on the skin or Streptococcus salivarius in the oral cavity. The Centers for Disease Control and Prevention (CDC) defines colonization as the presence of microbes without tissue invasion or damage, distinguishing it from infection (CDC, "Principles of Epidemiology in Public Health Practice," 3rd Edition, 2012).
Option B, "Infection," is incorrect because it involves the invasion and multiplication of pathogens in body tissues, leading to an immune response, such as inflammation, fever, or antibody production. This contrasts with the question’s description of no defense mechanism response. Option C, "Latency," refers to a state where a pathogen (e.g., herpes simplex virus or Mycobacterium tuberculosis) remains dormant in the body after initial infection, capable of reactivation but not eliciting an active immune response during dormancy. However, latency implies a prior infection with a latent phase, whereas the question suggests a current, non-responsive state without prior infection context. Option D, "Contamination," describes the unintended presence of pathogens on inanimate objects or surfaces (e.g., medical equipment), not within the body, and does not align with the scenario of living, culturable pathogens in a host.
The CBIC Practice Analysis (2022) and CDC guidelines highlight colonization as a key concept in infection control, particularly in settings like hospitals where colonized patients can serve as reservoirs for potential infections. The absence of an immune response, as specified, aligns with the definition of colonization, making Option A the most accurate answer.
Bioterrorism agents are classified according to priority. Which organism is listed as a Category A agent?
Q fever
Smallpox
Influenza
Brucellosis
The Certification Study Guide (6th edition) explains that bioterrorism agents are categorized by the Centers for Disease Control and Prevention (CDC) into Categories A, B, and C based on their potential impact on public health. Category A agents represent the highest priority because they pose a severe threat to national security and public health. These agents are characterized by ease of dissemination or transmission, high mortality rates, potential for major public health impact, and the ability to cause public panic and social disruption.
Smallpox (variola virus) is a classic and well-recognized Category A bioterrorism agent. The study guide emphasizes that although naturally occurring smallpox has been eradicated globally, the virus remains a major concern because the general population lacks immunity, person-to-person transmission is efficient, and outbreaks would require extensive public health response. Smallpox also necessitates strict isolation precautions and rapid vaccination strategies during suspected or confirmed cases.
The other options fall into lower categories. Q fever and brucellosis are classified as Category B agents, as they are moderately easy to disseminate but typically cause lower mortality rates. Influenza, while capable of causing pandemics, is not classified as a bioterrorism Category A agent.
Understanding bioterrorism classifications is essential for infection preventionists, particularly in emergency preparedness, surveillance, and response planning—key knowledge areas emphasized on the CIC exam.
Which of the following process performance indicators should result in improvement in central line–associated bloodstream infections (CLABSI)?
All patients with a central line are on total parenteral nutrition (TPN).
100% compliance with the insertion bundle.
Povidone-iodine antiseptic ointment placed at the insertion site of a peripherally inserted central catheter line.
Routinely changing the central line over a guidewire every seven days.
The Certification Study Guide (6th edition) emphasizes that process performance indicators directly linked to evidence-based practices are the most effective measures for reducing healthcare-associated infections such as CLABSI. Among the options listed, 100% compliance with the central line insertion bundle is the only indicator consistently demonstrated to reduce CLABSI rates.
Insertion bundles are standardized sets of practices that include proper hand hygiene, maximal sterile barrier precautions, use of appropriate skin antisepsis (preferably chlorhexidine), optimal catheter site selection, and daily review of line necessity. The study guide explains that reliable execution of these bundled practices addresses the most common routes of microbial entry at the time of line placement, which is a critical risk period for bloodstream infection.
The other options do not represent valid improvement indicators. Total parenteral nutrition is a known risk factor for CLABSI, not a prevention strategy. Use of povidone-iodine ointment at insertion sites is not recommended and may increase infection risk. Routine guidewire exchanges are discouraged because they do not reduce infection risk and may increase contamination.
Therefore, measuring and achieving full compliance with the insertion bundle is a meaningful, actionable performance indicator that aligns with CBIC exam expectations and infection prevention best practices.
A facility performs active surveillance cultures for methicillin-resistant Staphylococcus aureus (MRSA) on all patients upon admission and weekly. Twenty-two of the patients with positive cultures for MRSA were transferred from outlying facilities. The following MRSA data for a 3-month period are shown. Review of the data reveals which of the following is increasing?

Transmission of MRSA on the unit
Prevalence of MRSA at admission
Patients with MRSA infection
Compliance with collecting MRSA cultures
The table separates admission cultures from weekly cultures, which is a common surveillance approach to distinguish imported MRSA burden (present on admission) from healthcare acquisition (newly detected later). The admission culture percent positive rises over the three months: 14% (Feb) → 18% (Mar) → 19% (Apr). That pattern indicates an increasing admission prevalence (option B). NHSN MDRO surveillance methods describe admission prevalence as a proxy measure using admission-related data to quantify organisms present at the time of entry into a location/facility.
By contrast, weekly culture positivity—often used as a proxy for on-unit acquisition/transmission when admission screening is in place—decreases: 6% → 5.6% → 4%, so option A is not increasing. The dataset also does not provide information about MRSA infections versus colonization (so C cannot be concluded), nor does it provide a denominator for “compliance” (e.g., expected admissions/weekly screens completed), so D cannot be determined. This interpretation aligns with standard infection prevention use of MRSA surveillance data to track prevalence (burden) versus incidence/acquisition.
In an outbreak of probable foodborne illness, a group of individuals develops watery diarrhea 48 hours after eating imported shellfish. The MOST likely causative organism is:
Vibrio cholerae
Hepatitis A virus
Staphylococcus aureus
Listeria monocytogenes
The CBIC Certified Infection Control Exam Study Guide (6th edition) highlights that consumption of raw or undercooked shellfish, particularly imported shellfish, is a well-recognized risk factor for waterborne and foodborne Vibrio infections, including Vibrio cholerae. The organism thrives in warm coastal waters and can contaminate shellfish harvested from endemic or inadequately regulated regions.
The clinical presentation described—profuse watery diarrhea occurring approximately 48 hours after exposure—is classic for Vibrio cholerae. The organism produces cholera toxin, which causes rapid fluid secretion into the intestinal lumen, resulting in large-volume watery stools. The incubation period typically ranges from a few hours to five days, making a 48-hour onset highly consistent with this pathogen.
The other options are less likely based on incubation period and symptom profile. Hepatitis A virus has an incubation period of weeks and presents with jaundice rather than acute watery diarrhea. Staphylococcus aureus food poisoning causes rapid onset (1–6 hours) due to preformed toxin and is commonly associated with vomiting. Listeria monocytogenes typically causes invasive disease rather than acute watery diarrhea and has a longer incubation period.
For CIC® exam preparation, recognizing shellfish-associated watery diarrhea with short incubation as characteristic of Vibrio cholerae is essential, particularly in outbreak investigations involving imported seafood.
At a facility with 10.000 employees. 5,000 are at risk for bloodbome pathogen exposure. Over the past five years, 100 of the 250 needlestick injuries involved exposure to bloodborne pathogens, and 2% of exposed employees seroconverted. How many employees became infected?
1
2
5
10
To determine the number of employees who seroconverted (became infected) after a needlestick exposure, we use the given data:
Total Needlestick Injuries: 250
Needlestick Injuries Involving Bloodborne Pathogens: 100
Seroconversion Rate: 2%
Calculation:
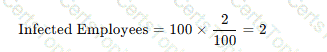
Why Other Options Are Incorrect:
A. 1: Incorrect calculation; 2% of 100 is 2, not 1.
C. 5: Overestimates the actual number of infections.
D. 10: Exceeds the calculated value based on given data.
CBIC Infection Control References:
APIC Text, "Occupational Exposure and Seroconversion Risks".
APIC Text, "Bloodborne Pathogens and Needlestick Injury Prevention"
Which of the following options describes a correct use of personal protective equipment?
Personal eyeglasses should be worn during suctioning.
Surgical masks should be worn during lumbar puncture procedures.
Gloves should be worn when handling or touching a cardiac monitor that has been disinfected.
Eye protection should be worn when providing patient care it at risk of spreading respiratory disease after unprotected exposure.
According to CDC and APIC guidelines, a surgical mask is required when performing lumbar punctures to prevent bacterial contamination (e.g., meningitis caused by droplet transmission of oral flora).
Why the Other Options Are Incorrect?
A. Personal eyeglasses should be worn during suctioning – Incorrect because eyeglasses do not provide adequate eye protection. Goggles or face shields should be used.
C. Gloves should be worn when handling or touching a cardiac monitor that has been disinfected – Not necessary unless recontamination is suspected.
D. Eye protection should be worn when providing patient care after unprotected exposure – Eye protection should be used before exposure, not just after.
CBIC Infection Control Reference
APIC states that surgical masks must be worn for procedures such as lumbar puncture to reduce infection risk.
An infection preventionist is asked to recommend a product for disinfection of bronchoscopes. Which of the following agents would be appropriate?
Iodophor
Alcohol
Phenolic
Peracetic acid
The correct answer is D, "Peracetic acid," as this agent is appropriate for the disinfection of bronchoscopes. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, bronchoscopes are semi-critical devices that require high-level disinfection (HLD) to eliminate all microorganisms except high levels of bacterial spores, as they come into contact with mucous membranes but not sterile tissues. Peracetic acid is recognized by the Centers for Disease Control and Prevention (CDC) and the Association for the Advancement of Medical Instrumentation (AAMI) as an effective high-level disinfectant for endoscopes, including bronchoscopes, due to its broad-spectrum antimicrobial activity, rapid action, and compatibility with the delicate materials (e.g., optics and channels) of these devices (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). It is commonly used in automated endoscope reprocessors, ensuring thorough disinfection when combined with proper cleaning and rinsing protocols.
Option A (iodophor) is typically used for intermediate-level disinfection and skin antisepsis, but it is not sufficient for high-level disinfection of bronchoscopes unless specifically formulated and validated for this purpose, which is uncommon. Option B (alcohol) is effective against some pathogens but evaporates quickly, fails to penetrate organic material, and is not recommended for HLD of endoscopes due to potential damage to internal components and inadequate sporicidal activity. Option C (phenolic) is suitable for surface disinfection but lacks the efficacy required for high-level disinfection of semi-critical devices like bronchoscopes, as it does not reliably eliminate all microbial threats, including mycobacteria.
The selection of peracetic acid aligns with CBIC’s emphasis on evidence-based reprocessing practices to prevent healthcare-associated infections (HAIs) associated with endoscope use (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.4 - Implement environmental cleaning and disinfection protocols). This choice ensures patient safety by adhering to manufacturer and regulatory guidelines, such as those in AAMI ST91 (AAMI ST91:2015, Flexible and semi-rigid endoscope processing in health care facilities).
Which of the following intravenous solutions will MOST likely promote the growth of microorganisms?
50% hypertonic glucose
5% dextrose
Synthetic amino acids
10% lipid emulsions
10% lipid emulsions are the most likely to promote microbial growth because they provide an ideal environment for bacterial and fungal proliferation, especially Staphylococcus aureus, Pseudomonas aeruginosa, and Candida species. Lipids support rapid bacterial multiplication due to their high nutrient content.
Why the Other Options Are Incorrect?
A. 50% hypertonic glucose – High glucose concentrations inhibit bacterial growth due to osmotic pressure effects.
B. 5% dextrose – While it can support some bacterial growth, it is less favorable than lipid emulsions.
C. Synthetic amino acids – These solutions do not support microbial growth as well as lipid emulsions.
CBIC Infection Control Reference
APIC guidelines confirm that lipid-based solutions support rapid microbial growth and should be handled with strict aseptic technique.
Which of the following study designs provides the STRONGEST evidence of a causal relationship between a risk factor and the outcome of interest?
Randomized clinical trial
Case-control study
Cohort study
Cross-sectional study
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies the randomized clinical trial (RCT) as the study design that provides the strongest evidence of a causal relationship between a risk factor (or intervention) and an outcome. RCTs are considered the gold standard because they use random assignment to allocate participants to either an intervention group or a control group, which minimizes bias and balances both known and unknown confounding variables between groups.
By controlling exposure and randomly assigning participants, RCTs establish temporality, ensuring that the exposure precedes the outcome—an essential criterion for causality. This design also allows for direct comparison of outcomes under controlled conditions, making it possible to attribute observed differences in outcomes to the intervention or risk factor with a high degree of confidence.
In contrast, cohort studies and case-control studies are observational and can identify associations but are more susceptible to confounding and bias. While cohort studies can demonstrate temporal relationships and estimate risk, they cannot control exposures as precisely as RCTs. Case-control studies are particularly vulnerable to recall and selection bias. Cross-sectional studies assess exposure and outcome simultaneously and cannot establish causation.
For the CIC® exam, it is critical to recognize that randomized clinical trials offer the highest level of evidence for causality, particularly when evaluating interventions, preventive measures, or treatment effectiveness in infection prevention and healthcare epidemiology.
An infection preventionist is reviewing a wound culture result on a surgery patient. The abdominal wound culture of purulent drainage grew Staphylococcus aureus with the following sensitivity pattern: resistant to penicillin, oxacillin, cephalothin, and erythromycin; susceptible to clindamycin, and vancomycin. The patient is currently being treated with cefazolin. Which of the following is true?
The wound is not infected.
The current therapy is not effective.
Droplet Precautions should be initiated.
This is a methicillin-sensitive S. aureus (MSSA) strain.
The scenario involves a surgical patient with a purulent abdominal wound culture growing Staphylococcus aureus, a common pathogen in surgical site infections (SSIs). The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes accurate interpretation of culture results and antibiotic therapy in the "Identification of Infectious Disease Processes" and "Prevention and Control of Infectious Diseases" domains, aligning with the Centers for Disease Control and Prevention (CDC) guidelines for managing SSIs. The question requires assessing the sensitivity pattern and current treatment to determine the correct statement.
Option B, "The current therapy is not effective," is true. The wound culture shows Staphylococcus aureus resistant to oxacillin, indicating methicillin-resistant S. aureus (MRSA). The sensitivity pattern lists resistance to penicillin, oxacillin, cephalothin, and erythromycin, with susceptibility to clindamycin and vancomycin. Cefazolin, a first-generation cephalosporin, is ineffective against MRSA because resistance to oxacillin (a penicillinase-resistant penicillin) implies cross-resistance to cephalosporins like cefazolin due to altered penicillin-binding proteins (PBPs). The CDC’s "Guidelines for the Prevention of Surgical Site Infections" (2017) and the Clinical and Laboratory Standards Institute (CLSI) standards confirm that MRSA strains are not susceptible to cefazolin, meaning the current therapy is inappropriate and unlikely to resolve the infection, supporting Option B.
Option A, "The wound is not infected," is incorrect. The presence of purulent drainage, a clinical sign of infection, combined with a positive culture for S. aureus, confirms an active wound infection. The CBIC and CDC define purulent discharge as a key indicator of SSI, ruling out this statement. Option C, "Droplet Precautions should be initiated," is not applicable. Droplet Precautions are recommended for pathogens transmitted via respiratory droplets (e.g., influenza, pertussis), not for S. aureus, which is primarily spread by contact. The CDC’s "Guideline for Isolation Precautions" (2007) specifies Contact Precautions for MRSA, not Droplet Precautions, making this false. Option D, "This is a methicillin-sensitive S. aureus (MSSA) strain," is incorrect. Methicillin sensitivity is determined by susceptibility to oxacillin, and the resistance to oxacillin in the culture result classifies this as MRSA, not MSSA. The CDC and CLSI use oxacillin resistance as the defining criterion for MRSA.
The CBIC Practice Analysis (2022) and CDC guidelines stress the importance of aligning antimicrobial therapy with sensitivity patterns to optimize treatment outcomes. The mismatch between cefazolin and the MRSA sensitivity profile confirms that Option B is the correct statement, indicating ineffective current therapy.
Each item or package that is prepared for sterilization should be labeled with the
storage location.
type of sterilization process.
sterilizer identification number or code.
cleaning method (e.g., mechanical or manual).
The correct answer is C, "sterilizer identification number or code," as this is the essential information that each item or package prepared for sterilization should be labeled with. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, proper labeling of sterilized items is a critical component of infection prevention and control to ensure traceability and verify the sterilization process. The sterilizer identification number or code links the item to a specific sterilization cycle, allowing the infection preventionist (IP) and sterile processing staff to track the equipment used, confirm compliance with standards (e.g., AAMI ST79), and facilitate recall or investigation if issues arise (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This labeling ensures that the sterility of the item can be assured and documented, protecting patient safety by preventing the use of inadequately processed items.
Option A (storage location) is important for inventory management but is not directly related to the sterilization process itself and does not provide evidence of the sterilization event. Option B (type of sterilization process) indicates the method (e.g., steam, ethylene oxide), which is useful but less critical than the sterilizer identification, as the process type alone does not confirm the specific cycle or equipment used. Option D (cleaning method, e.g., mechanical or manual) is a preliminary step in reprocessing, but it is not required on the sterilization label, as the focus shifts to sterilization verification once the item is prepared.
The requirement for a sterilizer identification number or code aligns with CBIC’s emphasis on maintaining rigorous tracking and quality assurance in the reprocessing of medical devices, ensuring accountability and adherence to best practices (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). This practice is mandated by standards such as AAMI ST79 to support effective infection control in healthcare settings.
The expectation to call out or speak up when an infection prevention lapse is observed is an example of
implementation of human factors.
honest disclosure of a safety event.
a blaming and shaming safety culture.
a safety culture with reciprocal accountability.
A safety culture with reciprocal accountability emphasizes mutual responsibility for maintaining safe practices, encouraging staff at all levels to "speak up" or "stop the line" when they observe risky practices. This concept reflects a learning organization and a just culture that supports open communication and proactive risk mitigation.
According to the APIC Text, a strong safety culture is described as one where:
“The leadership can expect staff members to call out or stop the line when they see risk, and staff can expect leadership to listen and act.”
This dynamic reflects reciprocal accountability.
Other options are less accurate:
A. Human factors refer to system design, not behavioral accountability.
B. Honest disclosure of a safety event is about post-event transparency, not real-time intervention.
C. A blaming and shaming culture is antithetical to safety culture principles.
Which of the following is an example of an outcome measure?
Hand hygiene compliance rate
Adherence to Environmental Cleaning
Rate of multi-drug resistant organisms acquisition
Timing of preoperative antibiotic administration
The correct answer is C, "Rate of multi-drug resistant organisms acquisition," as it represents an example of an outcome measure. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, outcome measures are indicators that reflect the impact or result of infection prevention and control interventions on patient health outcomes or the incidence of healthcare-associated infections (HAIs). The rate of multi-drug resistant organisms (MDRO) acquisition directly measures the incidence of new infections caused by resistant pathogens, which is a key outcome affected by the effectiveness of infection control practices (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.4 - Evaluate the effectiveness of infection prevention and control interventions).
Option A (hand hygiene compliance rate) is an example of a process measure, which tracks adherence to specific protocols or practices intended to prevent infections, rather than the resulting health outcome. Option B (adherence to environmental cleaning) is also a process measure, focusing on the implementation of cleaning protocols rather than the end result, such as reduced infection rates. Option D (timing of preoperative antibiotic administration) is another process measure, assessing the timeliness of an intervention to prevent surgical site infections, but it does not directly indicate the outcome (e.g., infection rate) of that intervention.
Outcome measures, such as the rate of MDRO acquisition, are critical for evaluating the success of infection prevention programs and are often used to guide quality improvement initiatives. This aligns with CBIC’s emphasis on using surveillance data to assess the effectiveness of interventions and inform decision-making (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.5 - Use data to guide infection prevention and control strategies). The focus on MDRO acquisition specifically highlights a significant healthcare challenge, making it a prioritized outcome measure in infection control.
Which of the following correctly characterizes endovaginal ultrasound probes?
They must be sterilized with a liquid chemical sterilant after use.
They are protected from viral contamination if covered by a sheath.
They are critical items based on the Spaulding Classification System.
They may be contaminated with human papillomavirus pre-examination.
The Certification Study Guide (6th edition) classifies endovaginal ultrasound probes as semi-critical devices because they come into contact with mucous membranes. As such, they require high-level disinfection (HLD) between patients, not sterilization, unless the manufacturer specifically requires it. This immediately eliminates option A, which incorrectly states sterilization is required.
Option B is incorrect because probe covers or sheaths do not eliminate the risk of contamination. Numerous studies referenced in infection prevention literature and reflected in the study guide demonstrate that probe covers can fail, tear, or leak, allowing microorganisms—including viruses—to contaminate the probe surface. Therefore, HLD is required regardless of sheath use.
Option C is incorrect because critical items, by definition, enter sterile tissue or the vascular system. Endovaginal probes contact mucous membranes only and are therefore not critical items under the Spaulding Classification System.
Option D is correct because endovaginal probes may be contaminated with human papillomavirus (HPV) prior to examination, even when probe covers are used. HPV is particularly concerning due to its resistance to some low-level disinfectants and its ability to persist on surfaces. The study guide highlights HPV as a key organism driving strict reprocessing requirements for these probes.
This question reflects a high-yield CIC exam concept: probe covers do not replace high-level disinfection, and viral contamination—including HPV—remains a significant risk.
A patient with shortness of breath and a history of a tuberculin skin test (TST) of 15 mm induration was admitted to a semi-private room. The infection preventionist's FIRST action should be to
contact the roommate's physician to initiate TST.
review the patient's medical record to determine the likelihood of pulmonary tuberculosis (TB).
report the findings to the Employee Health Department to initiate exposure follow-up of hospital staff.
transfer the patient to an airborne infection isolation room and initiate appropriate isolation for tuberculosis (TB).
Before initiating airborne precautions, the infection preventionist must first confirm the clinical suspicion of active TB.
Step-by-Step Justification:
Confirming Active TB:
A positive tuberculin skin test (TST) alone does not indicate active disease.
A review of chest X-ray, symptoms, and risk factors is needed.
Medical Record Review:
Past TB history, imaging, and sputum testing are key to diagnosis.
Not all TST-positive patients require isolation.
Why Other Options Are Incorrect:
A. Contact the roommate's physician to initiate TST: Premature, as no confirmation of active TB exists yet.
C. Report findings to Employee Health for staff follow-up: Should occur only after TB confirmation.
D. Transfer to airborne isolation immediately: Airborne isolation is necessary only if active TB is suspected based on clinical findings.
CBIC Infection Control References:
The Infection Control Department is notified of possible contamination of one lot of dressings. Which of the following actions should be taken?
Instruct the Purchasing Department to remove the manufacturer’s dressings and similar dressings from the hospital.
Notify discharged patients on whom the dressings were used to be alert for signs of infection.
Identify where the implicated dressings are in the hospital so that they can be returned to the manufacturer.
Arrange to purchase new dressings from a different manufacturer.
The Certification Study Guide (6th edition) emphasizes that when a specific product lot is suspected or confirmed to be contaminated, the first priority is containment and traceability. The infection preventionist must promptly identify where the implicated lot is located within the facility so it can be removed from use, quarantined, and managed according to recall or manufacturer instructions. This step prevents further patient exposure and preserves the ability to conduct an accurate risk assessment.
Locating the affected dressings allows the facility to determine how widely the product has been distributed, whether it is still in use, and which clinical areas may be affected. This information is essential before taking additional actions such as patient notification or broad product removal. The study guide stresses that responses must be proportionate and evidence-based, avoiding unnecessary disruption or alarm.
The other options represent actions that may be considered later, depending on findings. Removing all dressings from the same manufacturer is overly broad when only one lot is implicated. Notifying discharged patients is premature unless patient exposure and risk have been confirmed. Purchasing from a different manufacturer does not address the immediate need to control and investigate the current issue.
CIC exam questions often focus on sequencing of actions during product contamination events. Correctly identifying and isolating the affected product lot is the foundational step that enables safe, effective follow-up and regulatory compliance.
A patient with a non-crusted rash has boon diagnosed with Sarcoptes scabiei. The patient is treated with 5% permethrin and precautions are started. The precautions can be stopped
when the treatment cream is applied
when the bed linen is changed
24 hours after effective treatment
24 hours after the second treatment
For Sarcoptes scabiei (scabies), Contact Precautions should remain in place until 24 hours after effective treatment has been completed. The first-line treatment is 5% permethrin cream, which is applied to the entire body and left on for 8–14 hours before being washed off.
Why the Other Options Are Incorrect?
A. When the treatment cream is applied – The mite is still present and infectious until treatment has fully taken effect.
B. When the bed linen is changed – While changing linens is necessary, it does not indicate that the infestation has cleared.
D. 24 hours after the second treatment – Most cases require only one treatment with permethrin, though severe cases may need a second dose after a week.
CBIC Infection Control Reference
According to APIC guidelines, Contact Precautions can be discontinued 24 hours after effective treatment has been administered.
A patient presents with symptoms of meningitis. Two weeks ago, the patient ate from a cheese and meat tray and developed fever, muscle aches, and nausea the next day. Which of the following infectious agents should an infection preventionist consider as a cause of the patient’s symptoms?
Vibrio cholerae
Campylobacter jejuni
Clostridium perfringens
Listeria monocytogenes
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies Listeria monocytogenes as a significant foodborne pathogen capable of causing invasive disease, including meningitis. Listeria is uniquely associated with ready-to-eat foods, particularly soft cheeses, deli meats, pâtés, and meat trays—making the patient’s dietary history highly suggestive. Unlike many other foodborne organisms, Listeria can grow at refrigeration temperatures, increasing the risk of contamination in processed and stored foods.
The incubation period for invasive listeriosis can range from several days to weeks, which aligns with the timeline described. Early symptoms often include fever, myalgias, nausea, and gastrointestinal upset, followed by progression to meningitis or bloodstream infection, especially in high-risk populations such as older adults, pregnant individuals, neonates, and immunocompromised patients. The study guide emphasizes that Listeria is an important consideration when meningitis follows a compatible food exposure history.
The other organisms listed are primarily associated with self-limited gastrointestinal illness, not meningitis. Vibrio cholerae causes severe watery diarrhea; Campylobacter jejuni causes enteritis; and Clostridium perfringens causes toxin-mediated food poisoning with rapid onset diarrhea and abdominal cramping. None are typical causes of meningitis.
This question highlights a high-yield CIC exam concept: linking food exposure history to invasive pathogens, particularly Listeria monocytogenes, which requires prompt recognition and intervention.
==========
What rate is expressed by the number of patients who acquire infections over a specified time period divided by the population at risk of acquiring an infection during that time period?
Incidence rate
Disease specific
Point prevalence
Period prevalence
The incidence rate measures new cases of infection in a population over a defined time period using the formula:
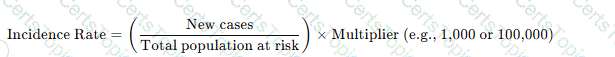
Why the Other Options Are Incorrect?
B. Disease specific – Refers to infections caused by a particular pathogen, not the general rate of new infections.
C. Point prevalence – Measures existing cases at a specific point in time, not new cases.
D. Period prevalence – Includes both old and new cases over a set period, unlike incidence, which only considers new cases.
CBIC Infection Control Reference
APIC defines incidence rate as the number of new infections in a population over a given period.
Passive immunity results from the use of:
Tetanus antitoxin
Hepatitis B vaccine
Influenza vaccine
Human diploid cell rabies vaccine
The Certification Study Guide (6th edition) defines passive immunity as protection that results from the administration of preformed antibodies, rather than stimulation of the individual’s own immune system. Passive immunity provides immediate but temporary protection, because the recipient does not produce antibodies and therefore does not develop immunologic memory.
Tetanus antitoxin is a classic example of passive immunity. It contains antibodies that neutralize tetanus toxin directly and is used in situations where immediate protection is needed, such as after certain wounds in individuals with unknown or inadequate vaccination history. The study guide emphasizes that passive immunization is particularly important in post-exposure management when waiting for an active immune response would be too slow to prevent disease.
The other options represent active immunization, not passive immunity. Vaccines such as hepatitis B vaccine, influenza vaccine, and human diploid cell rabies vaccine stimulate the recipient’s immune system to produce its own antibodies and immune memory. While rabies immune globulin provides passive immunity, the rabies vaccine itself is an active immunizing agent.
This distinction between active and passive immunity is a frequently tested CIC exam concept, especially in the context of occupational health, post-exposure prophylaxis, and immunization programs. Recognizing that passive immunity involves antibody products (antitoxins or immune globulins) rather than vaccines is essential for accurate infection prevention decision-making.
There has been an outbreak of foodborne illness in the community believed to be associated with attendance at a church festival. Which of the following is the MOST appropriate denominator for calculation of the attack rate?
People admitted to hospitals with gastrointestinal symptoms
Admission tickets sold to the festival
Dinners served at the festival
Residents in the county who attended the festival
The attack rate, a key epidemiological measure in outbreak investigations, is defined as the proportion of individuals who become ill after exposure to a suspected source, calculated as the number of cases divided by the population at risk. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes accurate outbreak analysis in the "Surveillance and Epidemiologic Investigation" domain, aligning with the Centers for Disease Control and Prevention (CDC) "Principles of Epidemiology in Public Health Practice" (3rd Edition, 2012). The question involves a foodborne illness outbreak linked to a church festival, requiring the selection of the most appropriate denominator to reflect the population at risk.
Option D, "Residents in the county who attended the festival," is the most appropriate denominator. The attack rate should be based on the total number of people exposed to the potential source of the outbreak (i.e., the festival), as this represents the population at risk for developing the foodborne illness. The CDC guidelines for foodborne outbreak investigations recommend using the number of attendees or participants as the denominator when the exposure is tied to a specific event, such as a festival. This approach accounts for all individuals who had the opportunity to consume the implicated food, providing a comprehensive measure of risk. Obtaining an accurate count of attendees may involve festival records, surveys, or estimates, but it directly reflects the exposed population.
Option A, "People admitted to hospitals with gastrointestinal symptoms," is incorrect as a denominator. This represents the number of cases (the numerator), not the total population at risk. Using cases as the denominator would invalidate the attack rate calculation, which requires a distinct population base. Option B, "Admission tickets sold to the festival," could serve as a proxy for attendees if all ticket holders attended, but it may overestimate the at-risk population if some ticket holders did not participate or underestimate it if additional guests attended without tickets. The CDC advises using actual attendance data when available, making this less precise than Option D. Option C, "Dinners served at the festival," is a potential exposure-specific denominator if the illness is linked to a particular meal. However, without confirmation that all cases are tied to a single dinner event (e.g., a specific food item), this is too narrow and may exclude attendees who ate other foods or did not eat but were exposed (e.g., via cross-contamination), making it less appropriate than the broader attendee count.
The CBIC Practice Analysis (2022) and CDC guidelines stress the importance of defining the exposed population accurately for attack rate calculations in foodborne outbreaks. Option D best captures the population at risk associated with festival attendance, making it the most appropriate denominator.
The MOST common reason for contamination of compounded pharmaceutical products is:
Direct touch by personnel
Inadequate laminar airflow
Infrequent environmental sampling
Inappropriate storage of pharmaceutical items
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies direct touch contamination by personnel as the most common cause of contamination of compounded pharmaceutical products. Human contact—particularly hands, gloves, sleeves, or improper manipulation of sterile components—is the greatest source of microbial contamination during compounding activities.
Even when engineering controls such as laminar airflow workbenches and cleanrooms are functioning correctly, contamination can occur if aseptic technique is not strictly followed. Touching sterile vial stoppers, syringe tips, needle hubs, or critical sites with nonsterile hands or gloves introduces microorganisms directly into the product. The Study Guide emphasizes that aseptic technique, hand hygiene, glove use, and competency validation are essential to preventing contamination.
Option B, inadequate laminar airflow, can contribute to contamination but is less common than direct touch errors and is usually detected through certification and monitoring. Option C, infrequent environmental sampling, does not cause contamination but may delay detection of problems. Option D, inappropriate storage, can affect product stability but is not the primary cause of contamination during compounding.
For CIC® exam preparation, it is critical to recognize that human factors are the leading source of contamination in sterile compounding. Infection prevention strategies therefore focus heavily on staff training, competency assessment, observation, and adherence to aseptic technique standards to reduce contamination risk.
As part of their antimicrobial stewardship initiative, Hospital A is using a qualitative study to assess their program. What type of data will be collected using this approach?
Numeric
Reliable
Reproducible
Subjective
Qualitative studies focus on collecting subjective data, including personal narratives, observations, and experiences. These data are not numeric, and instead aim to explore themes and meaning from contextual, non-quantifiable information.
From the APIC Text:
“Qualitative methods... Measures or data: Subjective, Unique, Differs over time, sample, and context.”
An infection preventionist has been asked to consult on disinfectant products for use in a long term care home. What should their primary concern be?
Patient care items are cleaned whenever visibly soiled.
An appropriate disinfectant should be available whenever items are used on patients known to be colonized with multi drug resistant organisms.
Disinfectant products should be compatible with the patient care devices used by the facility.
Disinfectant products should have a mild odor to reduce allergy concerns.
The most critical factor in choosing disinfectants in long-term care is compatibility with medical devices to prevent damage and ensure safety. Improper selection can compromise disinfection efficacy and equipment longevity.
The APIC/JCR Workbook highlights:
“Organizations should evaluate compatibility of disinfectant products with the materials used in patient care equipment. Incompatibility can lead to equipment degradation or malfunction”.
This ensures compliance with manufacturer instructions and preserves warranty and functionality.
When designing a physical construction containment barrier to contain dust as well as potentially infectious microorganisms generated, reduced air pressure in the contained space relative to adjacent occupied spaces results in airflow from the:
Exhaust into the contained work space and then into the clean adjacent space.
Contained work space into the clean adjacent space and then out of the exhaust.
Clean adjacent space into the contained work space and then out the exhaust.
Clean adjacent space into the contained work space and then directly back into the building.
The Certification Study Guide (6th edition) explains that during construction, renovation, or maintenance activities in healthcare facilities, negative (reduced) air pressure within the contained work area is a critical engineering control to prevent the spread of dust and potentially infectious microorganisms. When the pressure inside the containment is lower than in adjacent occupied areas, air naturally flows from areas of higher pressure to areas of lower pressure.
As a result, airflow moves from the clean adjacent space into the contained work space, rather than allowing contaminated air to escape outward. Once inside the containment, the air is then exhausted directly to the outside of the building or through appropriate filtration systems. This airflow pattern protects patients, visitors, and healthcare personnel in occupied areas by preventing construction-related contaminants—such as fungal spores (e.g., Aspergillus)—from spreading into patient care environments.
The study guide emphasizes that this principle is foundational to Infection Control Risk Assessments (ICRAs) and construction containment planning. Improper airflow direction can result in airborne contamination and has been associated with outbreaks, particularly among immunocompromised patients.
The incorrect options either reverse the airflow direction or allow contaminated air to re-enter the building, both of which violate infection prevention standards. Understanding airflow dynamics and pressure differentials is a frequently tested concept on the CIC exam and is essential for ensuring safe construction practices in healthcare facilities.
A hospital wants to launch an alternative care site due to an influx of patients from a mass casualty incident. An infection preventionist should be engaged to BEST determine:
Optimal medical care being offered.
Staffing of licensed and unlicensed staff.
Measures to keep all individuals healthy.
Requirements for providing direct patient care.
The Certification Study Guide (6th edition) outlines the critical role of the infection preventionist (IP) in emergency preparedness and response, particularly when healthcare systems activate alternate or alternative care sites during mass casualty incidents or public health emergencies. In these situations, the IP’s primary responsibility is to determine the infection prevention and control requirements necessary to safely provide direct patient care in nontraditional settings.
Alternate care sites often lack the infrastructure of acute care hospitals, such as standard ventilation, hand hygiene facilities, isolation rooms, or routine environmental services. The study guide emphasizes that infection preventionists must assess risks related to patient placement, cohorting, isolation precautions, environmental cleaning, waste management, water safety, and availability of personal protective equipment. These determinations directly influence whether patient care can be delivered safely and sustainably under emergency conditions.
The other options fall outside the IP’s primary scope. Decisions about optimal medical care and staffing models are led by clinical and administrative leadership. “Measures to keep all individuals healthy” is overly broad and does not reflect the IP’s focused, operational role during emergency site activation.
CIC exam questions frequently test understanding of role delineation during emergency management. The infection preventionist’s expertise is best applied to defining infection control standards and requirements that enable safe direct patient care—making option D the most accurate and appropriate answer.
Which of the following active surveillance screening cultures would be appropriate for carbapenem-resistant Enterobacterales (previously known as carbapenem-resistant Enterobacteriaceae) (CRE)?
Rectal or peri-rectal cultures
Nares or axillary cultures
Abscess or blood cultures
Throat or nasopharyngeal cultures
Carbapenem-resistant Enterobacterales (CRE) colonization is most commonly found in the gastrointestinal (GI) tract. Therefore, rectal or peri-rectal cultures are recommended for active surveillance screening.
Why the Other Options Are Incorrect?
B. Nares or axillary cultures – CRE is not primarily found in the nasal or axillary region; this method is more relevant for detecting MRSA.
C. Abscess or blood cultures – While CRE may be present in clinical infections, these cultures are not used for screening asymptomatic carriers.
D. Throat or nasopharyngeal cultures – CRE does not commonly colonize the upper respiratory tract, so these are not ideal for active screening.
CBIC Infection Control Reference
The CDC and APIC guidelines emphasize rectal or peri-rectal swabbing as the most effective active surveillance method for CRE detection.
In which of the following ways is human immunodeficiency virus similar to the Hepatitis B virus?
The primary mechanism of transmission for both is maternal-fetal
Needlestick exposure leads to a high frequency of healthcare worker infection
Transmission may occur from asymptomatic carriers
The risk of infection from mucous membrane exposure is the same
The human immunodeficiency virus (HIV) and Hepatitis B virus (HBV) are both bloodborne pathogens that pose significant risks in healthcare settings, and understanding their similarities is crucial for infection prevention and control. The Certification Board of Infection Control and Epidemiology (CBIC) emphasizes the importance of recognizing transmission modes and implementing appropriate precautions in the "Prevention and Control of Infectious Diseases" domain, aligning with guidelines from the Centers for Disease Control and Prevention (CDC). Comparing these viruses involves evaluating their epidemiology, transmission routes, and occupational risks.
Option C, "Transmission may occur from asymptomatic carriers," is the correct answer. Both HIV and HBV can be transmitted by individuals who are infected but show no symptoms, making asymptomatic carriage a significant similarity. For HBV, chronic carriers (estimated at 257 million globally per WHO, 2019) can transmit the virus through blood, semen, or other bodily fluids without overt signs of disease. Similarly, HIV-infected individuals can remain asymptomatic for years during the latent phase, yet still transmit the virus through sexual contact, blood exposure, or perinatal transmission. The CDC’s "Guidelines for Prevention of Transmission of HIV and HBV to Healthcare Workers" (1987, updated 2011) and "Epidemiology and Prevention of Viral Hepatitis" (2018) highlight this shared characteristic, underscoring the need for universal precautions regardless of symptom status.
Option A, "The primary mechanism of transmission for both is maternal-fetal," is incorrect. While maternal-fetal transmission (perinatal transmission) is a significant route for both HIV and HBV—occurring in 5-10% of cases without intervention for HBV and 15-45% for HIV without antiretroviral therapy—it is not the primary mechanism. For HBV, the primary mode is horizontal transmission through unprotected sexual contact or percutaneous exposure (e.g., needlesticks), accounting for the majority of cases. For HIV, sexual transmission and intravenous drug use are the leading modes globally, with maternal-fetal transmission being a smaller proportion despite its importance. Option B, "Needlestick exposure leads to a high frequency of healthcare worker infection," is partially true but not a precise similarity. Needlestick exposures carry a high risk for HBV (transmission risk ~30% if the source is HBeAg-positive) and a lower risk for HIV (~0.3%), but the frequency of infection among healthcare workers is significantly higher for HBV due to its greater infectivity and stability outside the host. This makes the statement more characteristic of HBV than a shared trait. Option D, "The risk of infection from mucous membrane exposure is the same," is false. The risk of HIV transmission via mucous membrane exposure (e.g., splash to eyes or mouth) is approximately 0.09%, while for HBV it is higher (up to 1-2% depending on viral load and exposure type), reflecting HBV’s greater infectivity.
The CBIC Practice Analysis (2022) and CDC guidelines emphasize the role of asymptomatic transmission in shaping infection control strategies, such as routine testing and post-exposure prophylaxis. This shared feature of HIV and HBV justifies Option C as the most accurate similarity.
A laboratory has received specimens labeled eye drainage for four patients. In preparing an action plan, the infection preventionist should do which of the following FIRST?
Cohort the patients based on the presence of eye drainage.
Monitor hand-washing practices of staff and visitors.
Determine the location of the patients.
Conduct pulsed-field gel electrophoresis.
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that when a potential cluster of infections is identified, the first priority is situational awareness. Before implementing control measures or advanced laboratory analysis, the infection preventionist must determine whether the cases are epidemiologically linked. Identifying the location of the patients—such as whether they are on the same unit, service, or clinic—is the essential first step in assessing the likelihood of transmission or a common source.
Option C is correct because determining patient location allows the IP to evaluate spatial and temporal relationships, which form the foundation of outbreak investigation. If the patients are colocated, this may indicate shared staff, equipment, or environmental exposure, guiding immediate and targeted interventions.
Cohorting patients (Option A) is premature without confirming proximity or transmission risk. Monitoring hand hygiene (Option B) is an important control measure but should follow confirmation of potential spread or shared risk factors. Pulsed-field gel electrophoresis (Option D) is an advanced molecular typing method and is never an initial step; it is reserved for later stages when epidemiologic evidence suggests related cases.
For the CIC® exam, this question tests understanding of outbreak investigation sequencing. The Study Guide consistently reinforces that defining who, where, and when comes before interventions or laboratory typing, making determination of patient location the correct first action.
The cleaning and disinfection process that is appropriate for a particular surgical instrument depends on
all surgical instruments are cleaned and sterilized in the same manner.
instruments contaminated with blood must be bleach cleaned first.
the device manufacturer's written instructions for use.
the policies of the sterile processing department.
The correct answer is C, "the device manufacturer's written instructions for use," as this is the factor that determines the appropriate cleaning and disinfection process for a particular surgical instrument. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the reprocessing of surgical instruments must follow the specific instructions provided by the device manufacturer to ensure safety and efficacy. These instructions account for the instrument’s material, design, and intended use, specifying the appropriate cleaning agents, disinfection methods, sterilization techniques, and contact times to prevent damage and ensure the elimination of pathogens (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). This is also mandated by regulatory standards, such as those from the Food and Drug Administration (FDA) and the Association for the Advancement of Medical Instrumentation (AAMI), which require adherence to manufacturer guidelines to maintain device integrity and patient safety.
Option A (all surgical instruments are cleaned and sterilized in the same manner) is incorrect because different instruments have unique characteristics (e.g., materials like stainless steel vs. delicate optics), necessitating tailored reprocessing methods rather than a one-size-fits-all approach. Option B (instruments contaminated with blood must be bleach cleaned first) is a misconception; while blood contamination requires thorough cleaning, bleach is not universally appropriate and may damage certain instruments unless specified by the manufacturer. Option D (the policies of the sterile processing department) may guide internal procedures but must be based on and subordinate to the manufacturer’s instructions to ensure compliance and effectiveness.
The emphasis on manufacturer instructions aligns with CBIC’s focus on evidence-based reprocessing practices to prevent healthcare-associated infections (HAIs) and protect patients (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.5 - Evaluate the environment for infection risks). Deviating from these guidelines can lead to inadequate sterilization or instrument damage, increasing infection risks.
There are four cases of ventilator-associated pneumonia in a surgical intensive care unit with a total of 200 ventilator days and a census of 12 patients. Which of the following BEST expresses how this should be reported?
Ventilator-associated pneumonia rate of 2%
20 ventilator-associated pneumonia cases/1000 ventilator days
Postoperative pneumonia rate of 6% in SICU patients
More information is needed regarding ventilator days per patient
The standard way to report ventilator-associated pneumonia (VAP) rates is:

Why the Other Options Are Incorrect?
A. Ventilator-associated pneumonia rate of 2% – This does not use the correct denominator (ventilator days).
C. Postoperative pneumonia rate of 6% in SICU patients – Not relevant, as the data focuses on VAP, not postoperative pneumonia.
D. More information is needed regarding ventilator days per patient – The total ventilator days are already provided, so no additional data is required.
CBIC Infection Control Reference
APIC and NHSN recommend reporting VAP rates as cases per 1,000 ventilator days.
An outbreak of Candida auris is suspected in the infection preventionist's (IP) facility. The IP's investigation must be conducted in a standard method and communication is critical. Which first step is MOST important?
Conduct environmental cultures
Plan to prevent future outbreaks
Notify facility administration
Perform analytical studies
In an outbreak investigation, the first critical step is to notify facility administration and other key stakeholders. This ensures the rapid mobilization of resources, coordination with infection control teams, and compliance with regulatory reporting requirements.
Why the Other Options Are Incorrect?
A. Conduct environmental cultures – While environmental sampling may be necessary, it is not the first step. The outbreak must first be confirmed and administration alerted.
B. Plan to prevent future outbreaks – Prevention planning happens later after the outbreak has been investigated and controlled.
D. Perform analytical studies – Data analysis occurs after case definition and initial response measures are in place.
CBIC Infection Control Reference
APIC guidelines state that the first step in an outbreak investigation is confirming the outbreak and notifying key stakeholders.
An HBsAb-negative employee has a percutaneous exposure to blood from a Hepatitis B surface antigen (HBsAg) positive patient. Which of the following regimens is recommended for this employee?
Immune serum globulin and hepatitis B vaccine
Hepatitis B immune globulin (HBIG) alone
Hepatitis B vaccine alone
Hepatitis B immune globulin (HBIG) and hepatitis B vaccine
The correct answer is D, "Hepatitis B immune globulin (HBIG) and hepatitis B vaccine," as this is the recommended regimen for an HBsAb-negative employee with a percutaneous exposure to blood from an HBsAg-positive patient. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, which align with recommendations from the Centers for Disease Control and Prevention (CDC) and the Advisory Committee on Immunization Practices (ACIP), post-exposure prophylaxis (PEP) for hepatitis B virus (HBV) exposure depends on the employee’s vaccination status and the source’s HBsAg status. For an unvaccinated or known HBsAb-negative individual (indicating no immunity) exposed to HBsAg-positive blood, the standard PEP includes both HBIG and the hepatitis B vaccine. HBIG provides immediate passive immunity by delivering pre-formed antibodies, while the vaccine initiates active immunity to prevent future infections (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents). The HBIG should be administered within 24 hours of exposure (preferably within 7 days), and the first dose of the vaccine should be given concurrently, followed by the complete vaccine series.
Option A (immune serum globulin and hepatitis B vaccine) is incorrect because immune serum globulin (ISG) is a general immunoglobulin preparation and not specific for HBV; HBIG, which contains high titers of anti-HBs, is the appropriate specific immunoglobulin for HBV exposure. Option B (hepatitis B immune globulin [HBIG] alone) is insufficient, as it provides only temporary passive immunity without initiating long-term active immunity through vaccination, which is critical for an unvaccinated individual. Option C (hepatitis B vaccine alone) is inadequate for immediate post-exposure protection, as it takes weeks to develop immunity, leaving the employee vulnerable in the interim.
The recommendation for HBIG and hepatitis B vaccine aligns with CBIC’s emphasis on evidence-based post-exposure management to prevent HBV transmission in healthcare settings (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.1 - Collaborate with organizational leaders). This dual approach is supported by CDC guidelines, which prioritize rapid intervention to reduce the risk of seroconversion following percutaneous exposure (CDC Updated U.S. Public Health Service Guidelines for the Management of Occupational Exposures to HBV, HCV, and HIV, 2013).
A review of bronchoscopy specimens indicates an unusual number of Mycobacterium fortuitum–positive cultures. Which of the following observations would be the MOST likely cause of this finding?
Bronchoscopes cleaned with sporicidal solution
Inadequate cleaning prior to disinfection
Rinsing with tap water
Drying with air or alcohol
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies nontuberculous mycobacteria (NTM), including Mycobacterium fortuitum, as organisms commonly associated with water sources, particularly potable water systems. An unusual increase in M. fortuitum–positive bronchoscopy cultures is most often linked to waterborne contamination during endoscope reprocessing, making rinsing with tap water the most likely cause.
Tap water is not sterile and may harbor NTM, which are resistant to standard municipal water treatment and capable of forming biofilms within plumbing systems. If bronchoscopes are rinsed with tap water after high-level disinfection and not followed by appropriate sterile or filtered water rinses and thorough drying, organisms such as M. fortuitum may contaminate internal channels. This can lead to pseudo-outbreaks, where cultures are positive due to contamination rather than true patient infection.
Option B, inadequate cleaning prior to disinfection, can contribute to overall reprocessing failure but is less specifically associated with NTM contamination patterns. Option A is unlikely, as sporicidal solutions are effective disinfectants. Option D, drying with air or alcohol, is a recommended step to reduce microbial growth and would not cause contamination.
For CIC® exam preparation, recognizing that tap water exposure during endoscope reprocessing is a classic source of nontuberculous mycobacteria contamination is a key concept in outbreak investigation and device reprocessing surveillance.
A city has a population of 150.000. Thirty new cases of tuberculosis (TB) were diagnosed in the city last year. These now cases brought the total number of active TB cases in the city last year to 115. Which of the following equations represents the incidence rate tor TB per 100.000 in that year?
(30 ÷ 150.000) x 100.000 = X
(30÷ 150.000) x 100 = X
(115 ÷ 150.000) x 100.000 - X
(115 ÷ 100.000) x 100 = X
The incidence rate is calculated using the formula:
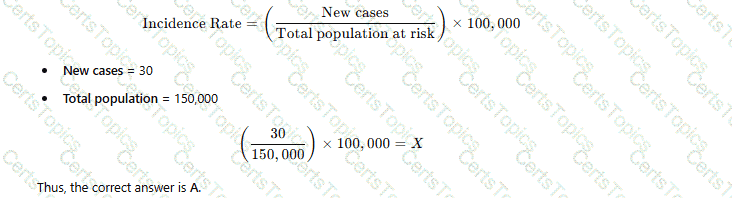

Why the Other Options Are Incorrect?
B. (30 ÷ 150,000) × 100 = X – Incorrect multiplier (should be 100,000 for standard incidence rate).
C. (115 ÷ 150,000) × 100,000 = X – 115 represents total cases (prevalence), not incidence.
D. (115 ÷ 100,000) × 100 = X – Uses the wrong denominator and multiplier.
CBIC Infection Control Reference
APIC defines the incidence rate as the number of new cases per population unit, typically per 100,000 people.
An infection preventionist is assisting the Product Evaluation Committee in selecting a disinfectant for use in a healthcare facility. Which of the following criteria is MOST important?
If it will be used on living tissue
The purpose for which it will be used
Active chemical ingredients
Safety Data Sheet (SDS)
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that the most important criterion when selecting a disinfectant is the intended purpose for which it will be used. Disinfectants must be chosen based on the type of surface or item, the level of microbial kill required, and the risk of infection associated with the use of that item. This approach aligns with Spaulding’s classification system, which categorizes items as critical, semi-critical, or noncritical and guides the required level of disinfection or sterilization.
Understanding the purpose of the disinfectant ensures that the selected product is effective against the appropriate microorganisms and suitable for the clinical application, whether it involves environmental surfaces, noncritical patient care equipment, or semi-critical devices. For example, a low-level disinfectant may be sufficient for noncritical items, whereas high-level disinfection is required for semi-critical devices. Selecting a disinfectant without first defining its purpose can result in ineffective infection prevention or unnecessary exposure to harsh chemicals.
Option A is incorrect because disinfectants are not intended for use on living tissue; antiseptics serve that role. Option C is secondary—while active ingredients matter, they are evaluated after determining intended use. Option D is important for safety and regulatory compliance but does not drive appropriateness of clinical application.
For the CIC® exam, recognizing that intended use is the foundational decision point in disinfectant selection is essential for evidence-based infection prevention practice.
Which of the following BEST describes the content of an interpretive surveillance report?
Outlines the organization’s mission for patient quality and safety
Cites the frequency of the evaluation of the monitoring program
Highlights the steps of the facility’s quality improvement activities
Provides findings in a manner designed for the intended audience
The CBIC Certified Infection Control Exam Study Guide (6th edition) explains that an interpretive surveillance report goes beyond simply presenting raw data. Its primary purpose is to translate surveillance findings into meaningful, actionable information that can be understood and used by the intended audience, such as frontline staff, clinical leaders, executive leadership, or quality committees.
Interpretive reports contextualize infection data by explaining trends, comparisons, implications, and recommended actions. This may include highlighting increases or decreases in infection rates, identifying areas of concern, interpreting statistical significance, and linking findings to prevention strategies. The format, level of detail, and language are tailored to the audience’s role and decision-making responsibilities. For example, senior leadership may need high-level summaries and risk implications, while unit-level staff benefit from detailed, practice-focused feedback.
Option A describes a mission statement, not a surveillance report. Option B refers to program evaluation logistics rather than interpretation of findings. Option C outlines quality improvement processes but does not describe how surveillance data are communicated.
For the CIC® exam, it is essential to recognize that interpretive surveillance reporting focuses on meaningful communication, not just data display. Providing findings in a manner designed for the intended audience ensures surveillance data drive prevention actions, accountability, and performance improvement—making option D the best answer.
In a busy family practice clinic, a patient has been diagnosed with measles solely on the basis of their rash. Upon investigation, the infection preventionist (IP) learns the family waited for 20 minutes in the waiting room, unmasked. What is the IP’s NEXT step?
Contact Public Health
Start a contact tracing
Discuss necessary testing with provider
Confirm immunization status and presence of other symptoms
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that measles is a reportable, airborne disease, but actions such as public health notification and contact tracing should occur after appropriate clinical and laboratory confirmation is initiated, unless there is a clear epidemiologic link or high clinical suspicion.
In this scenario, the diagnosis was made solely on the basis of rash, which is insufficient to confirm measles. Many viral illnesses can present with rash, and misclassification can lead to unnecessary alarm, resource use, and disruption. Therefore, the next appropriate step for the infection preventionist is to discuss necessary diagnostic testing with the provider, such as measles-specific IgM serology and PCR testing, to confirm or rule out measles.
Options A and B are premature. Public health notification and contact tracing are essential after measles is suspected and testing is initiated or confirmed, but they should not precede diagnostic clarification when the diagnosis is uncertain. Option D may support clinical assessment but does not replace the need for laboratory confirmation.
The Study Guide highlights that infection preventionists must balance rapid response with diagnostic accuracy. Ensuring appropriate testing is initiated first allows subsequent infection control actions—such as airborne exposure assessment and public health reporting—to be targeted, evidence-based, and defensible.
For the CIC® exam, this question tests understanding of sequencing infection prevention actions, reinforcing that confirmation and testing discussion is the critical next step before escalation.
During an outbreak of ventilator-associated pneumonia (VAP), the infection preventionist should FIRST:
Review adherence to ventilator bundle elements.
Implement preemptive antibiotic therapy in all ventilated patients.
Isolate all ventilated patients in negative pressure rooms.
Perform bacterial cultures from ventilator circuits.
Reviewing compliance with VAP prevention bundles (e.g., head-of-bed elevation, oral care, sedation breaks) is the first step in outbreak control.
Preemptive antibiotics (B) are not recommended due to antibiotic resistance risks.
Negative pressure rooms (C) are not required for VAP.
Ventilator circuit cultures (D) do not guide patient management.
CBIC Infection Control References:
APIC Text, "VAP Prevention Measures," Chapter 11.
Which of the following is the BEST strategy for reducing bloodstream infections associated with central venous catheters?
Routine replacement of central lines every 7 days.
Use of chlorhexidine-impregnated dressings.
Daily blood cultures for patients with central lines.
Use of povidone-iodine instead of chlorhexidine for skin antisepsis.
Chlorhexidine-impregnated dressings reduce central line-associated bloodstream infections (CLABSI) by preventing bacterial colonization.
Routine catheter replacement (A) increases insertion risks without reducing infections.
Daily blood cultures (C) are unnecessary and lead to false positives.
Povidone-iodine (D) is less effective than chlorhexidine for skin antisepsis.
CBIC Infection Control References:
APIC Text, "CLABSI Prevention Measures," Chapter 10.
Which of the following should be included when designing a data collection form for surveillance?
Denominator information
Only the information needed
As much information as possible
Medication history
The Certification Study Guide (6th edition) emphasizes that effective surveillance depends on the ability to calculate rates, not just counts. To calculate any infection rate, both a numerator (number of infection events) and a denominator (population at risk or time at risk) are required. Therefore, inclusion of denominator information is essential when designing a data collection form for surveillance.
Denominator data may include patient days, device days (e.g., central line days, ventilator days), number of procedures, or number of admissions—depending on the surveillance objective. Without denominator data, infection preventionists cannot calculate standardized rates, compare trends over time, or benchmark against national databases. The study guide clearly states that surveillance systems lacking denominator data produce incomplete and potentially misleading results.
The other options are either vague or inappropriate. While data collection forms should avoid unnecessary information, simply stating “only the information needed” does not address the critical requirement for denominator data. Collecting “as much information as possible” is discouraged because it increases workload, reduces data quality, and may compromise sustainability of surveillance programs. Medication history is not routinely required for most surveillance activities unless it is directly related to the infection being studied.
This question reflects a fundamental CIC exam principle: surveillance must be designed to support valid rate calculation and analysis. Including denominator information ensures that collected data are meaningful, actionable, and aligned with evidence-based infection prevention practices.
Which of the following infectious diseases is associated with environmental fungi?
Listeriosis
Hantavirus
Mucormycosis
Campylobacter
The correct answer is C, "Mucormycosis," as it is the infectious disease associated with environmental fungi. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, mucormycosis is caused by fungi belonging to the order Mucorales, which are commonly found in the environment, including soil, decaying organic matter, and contaminated water. These fungi can become opportunistic pathogens, particularly in immunocompromised individuals, leading to severe infections such as rhinocerebral, pulmonary, or cutaneous mucormycosis (CBIC Practice Analysis, 2022, Domain I: Identification of Infectious Disease Processes, Competency 1.1 - Identify infectious disease processes). Environmental exposure, such as inhalation of fungal spores or contact with contaminated materials, is a primary mode of transmission, making it directly linked to environmental fungi.
Option A (Listeriosis) is caused by the bacterium Listeria monocytogenes, typically associated with contaminated food products (e.g., unpasteurized dairy or deli meats) rather than environmental fungi. Option B (Hantavirus) is a viral infection transmitted through contact with rodent excreta, not fungi, and is linked to environmental reservoirs like rodent-infested areas. Option D (Campylobacter) is a bacterial infection caused by Campylobacter species, often associated with undercooked poultry or contaminated water, and is not related to fungi.
The association of mucormycosis with environmental fungi underscores the importance of infection prevention strategies, such as controlling environmental contamination and protecting vulnerable patients, which aligns with CBIC’s focus on identifying and mitigating risks from infectious agents in healthcare settings (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents). This knowledge is critical for infection preventionists to guide environmental cleaning and patient care protocols.
Which of the following community-acquired infections has the greatest potential public health impact?
Cryptosporidium enteritis
Fifth disease (parvovirus B-19)
Clostridial myositis (gas gangrene)
Cryptococcal meningitis
The correct answer is A, "Cryptosporidium enteritis," as it has the greatest potential public health impact among the listed community-acquired infections. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, the public health impact of an infection is determined by factors such as its transmissibility, severity, population at risk, and potential for outbreaks. Cryptosporidium enteritis, caused by the protozoan parasite Cryptosporidium, is a waterborne illness that spreads through contaminated water or food, leading to severe diarrhea, particularly in immunocompromised individuals. Its significant public health impact stems from its high transmissibility in community settings (e.g., via recreational water or daycare centers), the difficulty in eradicating the oocysts with standard chlorination, and the potential to cause large-scale outbreaks affecting vulnerable populations, such as children or the elderly (CBIC Practice Analysis, 2022, Domain I: Identification of Infectious Disease Processes, Competency 1.3 - Apply principles of epidemiology). This is exemplified by notable outbreaks, such as the 1993 Milwaukee outbreak affecting over 400,000 people.
Option B (Fifth disease, caused by parvovirus B-19) is a viral infection primarily affecting children, causing a mild rash and flu-like symptoms. While it can pose risks to pregnant women (e.g., fetal anemia), it is generally self-limiting and has limited community-wide transmission potential, reducing its public health impact. Option C (clostridial myositis, or gas gangrene, caused by Clostridium perfringens) is a severe but rare infection typically associated with traumatic wounds or surgery, with limited person-to-person spread, making its public health impact low due to its sporadic nature. Option D (cryptococcal meningitis, caused by Cryptococcus neoformans) primarily affects immunocompromised individuals (e.g., those with HIV/AIDS) and is not highly transmissible in the general community, confining its impact to specific at-risk groups rather than the broader population.
The selection of Cryptosporidium enteritis aligns with CBIC’s focus on identifying infections with significant epidemiological implications, enabling infection preventionists to prioritize surveillance and control measures for diseases with high outbreak potential (CBIC Practice Analysis, 2022, Domain II: Surveillance and Epidemiologic Investigation, Competency 2.1 - Conduct surveillance for healthcare-associated infections and epidemiologically significant organisms). This is supported by CDC data highlighting waterborne pathogens as major public health concerns (CDC Parasites - Cryptosporidium, 2023).
Education and training on safe work practices should be
Specific to a job or task.
Optional at the time of orientation.
Conducted in the nationally approved language.
Provided when policies and procedures are reviewed.
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that education and training on safe work practices must be specific to the job or task performed. This principle aligns with occupational safety and infection prevention standards, which recognize that risks vary significantly depending on an employee’s role, responsibilities, and work environment. Training is most effective when it directly addresses the actual hazards staff may encounter and the specific procedures they are expected to perform.
Job- and task-specific training ensures that healthcare personnel understand how to apply safe practices in real-world situations, such as proper use of personal protective equipment, safe handling of sharps, device reprocessing, and exposure prevention. Generic or overly broad education may fail to address critical nuances and can result in gaps in compliance or increased risk of injury and infection.
Option B is incorrect because safety education is not optional and must be provided at orientation and ongoing as needed. Option C is misleading; while training should be provided in a language and format the employee understands, there is no concept of a single “nationally approved language.” Option D describes a possible timing for education but does not capture the core requirement that training be tailored to specific work activities.
For the CIC® exam, this question reinforces that effective infection prevention and occupational safety education must be job- and task-specific, making option A the correct answer.
Which of the following control measures is MOST effective in preventing transmission of Legionella in healthcare water systems?
Flushing all faucets with hot water for 5 minutes daily.
Maintaining hot water storage temperatures above 140°F (60°C).
Installing carbon filters on all hospital water outlets.
Routine testing for Legionella in hospital water.
Maintaining hot water at 140°F (60°C) prevents Legionella growth and is the most effective control strategy.
Flushing water (A) alone is not sufficient.
Carbon filters (C) do not remove Legionella.
Routine testing (D) is not always necessary unless an outbreak occurs.
CBIC Infection Control References:
APIC Text, "Waterborne Pathogens and Infection Control," Chapter 9.
Which of the following management activities should be performed FIRST?
Evaluate project results
Establish goals
Plan and organize activities
Assign responsibility for projects
To determine which management activity should be performed first, we need to consider the logical sequence of steps in effective project or program management, particularly in the context of infection control as guided by CBIC principles. Management activities typically follow a structured process, and the order of these steps is critical to ensuring successful outcomes.
A. Evaluate project results: Evaluating project results involves assessing the outcomes and effectiveness of a project after its implementation. This step relies on having completed the project or at least reached a stage where outcomes can be measured. Performing this activity first would be premature, as there would be no results to evaluate without prior planning, goal-setting, and execution. Therefore, this cannot be the first step.
B. Establish goals: Establishing goals is the foundational step in any management process. Goals provide direction, define the purpose, and set the criteria for success. In the context of infection control, as emphasized by CBIC, setting clear objectives (e.g., reducing healthcare-associated infections by a specific percentage) is essential before any other activities can be planned or executed. This step aligns with the initial phase of strategic planning, making it the logical first activity. Without established goals, subsequent steps lack focus and purpose.
C. Plan and organize activities: Planning and organizing activities involve developing a roadmap to achieve the goals, including timelines, resources, and tasks. This step depends on having clear goals to guide the planning process. In infection control, this might include designing interventions to meet infection reduction targets. While critical, it cannot be the first step because planning requires a predefined objective to be effective.
D. Assign responsibility for projects: Assigning responsibility involves delegating tasks and roles to individuals or teams. This step follows the establishment of goals and planning, as responsibilities need to be aligned with the specific objectives and organized activities. In an infection control program, this might mean assigning staff to monitor compliance with hand hygiene protocols. Doing this first would be inefficient without a clear understanding of the goals and plan.
The correct sequence in management, especially in a structured field like infection control, begins with establishing goals to provide a clear target. This is followed by planning and organizing activities, assigning responsibilities, and finally evaluating results. The CBIC framework supports this approach by emphasizing the importance of setting measurable goals as part of the infection prevention and control planning process, which is a prerequisite for all subsequent actions.
CBIC Infection Prevention and Control (IPC) Core Competency Model (updated 2023), Domain V: Management and Communication, which highlights the importance of setting goals as the initial step in managing infection control programs.
CBIC Examination Content Outline, Domain V: Leadership and Program Management, which underscores the need for goal-setting prior to planning and implementation of infection control initiatives.
Which of the following is NOT valuable when using a graph to display data?
Title with topic of data
Facility and time frame for data
Published trends for data comparison
X and Y axes labels and annotation where indicated
The Certification Study Guide (6th edition) explains that graphs are most effective when they clearly communicate who, what, when, and how regarding the data being presented. Essential elements include a descriptive title, identification of the facility and time frame, and properly labeled X and Y axes with annotations as needed. These components ensure that the viewer can accurately interpret the data without additional explanation.
Published trends for data comparison, while potentially useful in separate analyses or reports, are not required elements of an individual graph and do not inherently improve the clarity of data display. Including external published trends can actually confuse interpretation if definitions, populations, or surveillance methodologies differ from the local data being presented. The study guide cautions against mixing datasets with different assumptions or collection methods in a single visual display unless clearly contextualized.
Titles clarify the subject of the graph, facility and time frame provide essential context, and axis labels ensure the viewer understands what is being measured. These are foundational principles of data visualization emphasized in infection prevention reporting and communication.
CIC exam questions frequently test the ability to distinguish between essential graph components and supplementary analytical tools. Recognizing that published comparison trends are not required—and may be misleading—reinforces good data communication practices and supports accurate interpretation by leadership and frontline staff.
An infection preventionist (IP) is asked to evaluate a series of published sources about CAUTI prevention strategies. Which source shows the strongest evidence for the IP to implement change?
A randomized controlled trial from another hospital
Evidence from reports written by authorities who are on expert committees
Data from a case study from a well-designed case-control or cohort study
A systematic review of relevant controlled studies and evidence-based practices
When an IP is selecting evidence to support practice change, the “strength” of evidence is typically judged using an evidence hierarchy. In most evidence pyramids, systematic reviews (often with meta-analysis) of well-designed studies sit at or near the top because they use explicit methods to search for, appraise, and synthesize findings across multiple studies—reducing the influence of chance results and individual-study bias.
Option D is therefore strongest: a systematic review of relevant controlled studies and evidence-based practices provides the most robust overall summary for decision-making compared with any single study. Randomized controlled trials (option A) are strong primary studies, but they represent one setting/population and can be affected by local factors; a high-quality systematic review places RCTs in context and evaluates consistency across multiple trials.
Observational designs (option C, cohort/case-control) are generally lower in the hierarchy for intervention effectiveness due to confounding risk, and expert committee reports (option B) are typically considered lower-level evidence unless they are explicitly based on systematic evidence review methods. For implementing CAUTI prevention changes, relying first on systematic syntheses best supports standardized, evidence-based practice.
A healthcare worker experiences a percutaneous exposure to a patient with untreated HIV. The next step is to:
Initiate HIV post-exposure prophylaxis (PEP) within 2 hours.
Wait for HIV test results before starting treatment.
Offer post-exposure prophylaxis only if symptoms develop.
Retest for HIV after 6 months before deciding on PEP.
HIV post-exposure prophylaxis (PEP) should be initiated within 2 hours to be most effective.
Waiting for results (B) delays critical treatment.
PEP should always be offered after high-risk exposure, not only if symptoms develop (C).
Retesting after 6 months (D) is recommended but should not delay PEP initiation.
CBIC Infection Control References:
APIC Text, "Bloodborne Pathogens and PEP," Chapter 11.
Passive immunity results from the use of:
Tetanus antitoxin.
Hepatitis B vaccine.
Influenza vaccine.
Human diploid cell rabies vaccine.
Passive immunity occurs when a person receives preformed antibodies (or antitoxin) made by another human or animal source. It provides immediate protection, but it is temporary because the transferred antibodies decline over weeks to months. CDC’s Pink Book defines passive immunity as protection by antibody or antitoxin produced by one individual and transferred to another.
Option A (tetanus antitoxin) is a classic example of passive immunization: antitoxin (including human tetanus immune globulin preparations) provides antibodies that neutralize tetanus toxin, giving rapid, short-term protection. CDC’s vaccine best-practices glossary notes that antitoxins are used to confer passive immunity.
In contrast, options B, C, and D are vaccines, which induce active immunity by stimulating the recipient’s immune system to produce its own antibodies and immune memory. That response takes time to develop but is longer-lasting than passive immunity.
An infection preventionist is writing a policy about prevention of intravascular device infection. Which of the following is important for healthcare personnel to know as part of central line insertion and maintenance procedures?
Change the central line every seven days.
Use maximum sterile barrier precautions for the line insertion.
The femoral site is the preferred site of insertion in an adult patient.
Use 70% isopropyl alcohol for skin preparation before line insertion.
The Certification Study Guide (6th edition) identifies the use of maximum sterile barrier (MSB) precautions during central line insertion as a cornerstone practice for preventing intravascular device–associated infections, including central line–associated bloodstream infections (CLABSIs). MSB precautions include wearing a cap, mask, sterile gown, and sterile gloves, and using a large sterile drape to fully cover the patient during line insertion. These measures significantly reduce the risk of introducing skin flora and environmental microorganisms into the bloodstream at the time of catheter placement.
The study guide emphasizes that the highest risk for contamination occurs during insertion, making strict aseptic technique essential. MSB precautions are a required element of evidence-based central line insertion bundles and are consistently associated with reduced CLABSI rates when reliably implemented.
The other options reflect outdated or incorrect practices. Routine scheduled replacement of central lines every seven days is not recommended and does not reduce infection risk. The femoral vein is not the preferred insertion site in adults due to higher infection risk compared to subclavian or internal jugular sites. While alcohol is used during hub disinfection, chlorhexidine-based antisepsis (preferably chlorhexidine with alcohol) is recommended for skin preparation—not alcohol alone.
This question highlights a core CIC exam concept: standardized insertion practices using maximum sterile barriers are among the most effective strategies for preventing intravascular device infections.
One of the elements of antibiotic stewardship is controlling antibiotic use. Which of the following BEST describes a closed formulary?
Requires the prescribing physician to obtain some form of approval before the antibiotic will be dispensed.
Automatic switching from broad-spectrum empiric therapy to narrower-spectrum agents.
Practice of rotating two or more classes of formulary drugs on a regular basis.
Limits the number of antibiotics available for physicians to prescribe.
Antibiotic stewardship programs are designed to optimize antimicrobial use, improve patient outcomes, reduce antimicrobial resistance, and decrease unnecessary costs. The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies formulary restriction and preauthorization as key core strategies within effective antimicrobial stewardship programs. A closed formulary specifically refers to a system in which access to certain antibiotics is restricted and requires prior approval before dispensing.
In a closed formulary model, prescribers must obtain authorization—often from infectious diseases specialists, pharmacy, or an antimicrobial stewardship team—before selected antimicrobial agents can be used. This approach ensures that high-risk, broad-spectrum, or high-cost antibiotics are used only when clinically appropriate. By requiring approval, the organization promotes judicious antibiotic selection, prevents unnecessary exposure, and supports resistance prevention efforts.
Option B describes de-escalation, which is another stewardship strategy but does not define a closed formulary. Option C refers to antibiotic cycling, a controversial and less-supported strategy. Option D is incorrect because a closed formulary does not merely limit availability; rather, it controls access through approval mechanisms.
For the CIC® exam, it is critical to distinguish between stewardship strategies. A closed formulary is best characterized by mandatory approval prior to dispensing, making option A the most accurate answer according to the Study Guide’s antimicrobial stewardship framework.
==========
An infection preventionist is putting together an educational program for families of patients newly diagnosed with Clostridioides difficile infection (CDI). Which of the following educational formats would involve active learning?
Providing a brief 10-minute lecture on ways to prevent CDI transmission
Distributing a pamphlet describing ways to prevent CDI transmission
Watching a 5-minute YouTube video demonstrating ways to prevent CDI transmission
Having the family members demonstrate ways to prevent CDI transmission
The correct answer is D, "Having the family members demonstrate ways to prevent CDI transmission," as this educational format involves active learning. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, active learning engages learners through participation, practice, and application of knowledge, which is more effective for skill development and behavior change compared to passive methods. In this context, having family members demonstrate techniques—such as proper hand hygiene, use of personal protective equipment (PPE), or environmental cleaning—requires them to actively apply the information, reinforcing understanding and retention (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.1 - Develop and implement educational programs). This hands-on approach also allows the infection preventionist to provide immediate feedback, ensuring correct practices to prevent CDI transmission, which is critical given the spore-forming nature of Clostridioides difficile.
Option A (providing a brief 10-minute lecture on ways to prevent CDI transmission) is a passive learning method where information is delivered to the audience without requiring their active participation, limiting its effectiveness for skill-based learning. Option B (distributing a pamphlet describing ways to prevent CDI transmission) is also passive, relying on the family to read and interpret the material independently, which may not ensure comprehension or application. Option C (watching a 5-minute YouTube video demonstrating ways to prevent CDI transmission) is a more engaging passive method, as it provides visual and auditory learning, but it still lacks the interactive component of active participation or demonstration.
The focus on active learning aligns with CBIC’s emphasis on tailoring educational programs to promote practical skills and sustained behavior change, which is essential for infection prevention among families of CDI patients (CBIC Practice Analysis, 2022, Domain IV: Education and Research, Competency 4.2 - Evaluate the effectiveness of educational programs). This approach supports the goal of reducing transmission risks in both healthcare and home settings.
The effectiveness of disinfection is NOT dependent upon the:
Virulence of the organism
Amount of organic material present
Spore-forming ability of the organism
Length of exposure to the chemical agent
The CBIC Certified Infection Control Exam Study Guide (6th edition) explains that the effectiveness of disinfection depends on multiple physical, chemical, and biologic factors, but virulence of the organism is not one of them. Virulence refers to an organism’s ability to cause disease in a host, which is a clinical characteristic, not a determinant of susceptibility to disinfectants.
Disinfection efficacy is influenced by factors such as the type and number of microorganisms, particularly their intrinsic resistance (for example, spores are more resistant than vegetative bacteria), making option C a true determinant. The amount of organic material present (option B) is also critical, as organic matter can inactivate disinfectants or shield microorganisms from exposure. Likewise, the length of exposure (contact time) to the chemical agent (option D) is essential to achieving the desired level of microbial kill and is specified in manufacturer instructions for use.
Virulence does not affect how easily an organism is destroyed by a disinfectant. For example, a highly virulent organism may be easily killed by a low-level disinfectant, while a less virulent organism such as a bacterial spore may be highly resistant. Therefore, virulence plays no role in determining disinfection effectiveness.
For CIC® exam preparation, it is important to distinguish between clinical severity and microbial resistance. Disinfection effectiveness is based on resistance characteristics and process variables—not on how dangerous the organism is to humans.
After reviewing quarterly surveillance data, the infection preventionist (IP) identifies an upward trend in needlestick injuries occurring during bedside blood draws. What is the MOST appropriate collaborative action for the IP to take with the Occupational Health Department?
Wait for the next regulatory survey to address the issue more formally with hospital leadership.
Complete a device review and determine if faulty equipment has been the cause or if the manufacturer has issued a recall.
Convene a multidisciplinary safety team to evaluate workflows, review device usage, and recommend practice changes.
Discuss trends at the quarterly quality assurance and performance improvement meeting with the multidisciplinary safety team.
The CBIC Certified Infection Control Exam Study Guide (6th edition) emphasizes that when surveillance identifies an increasing trend in occupational exposures, such as needlestick injuries, the infection preventionist must take prompt, proactive, and collaborative action. The most appropriate response is to convene a multidisciplinary safety team in partnership with Occupational Health to perform a focused evaluation of the problem.
A multidisciplinary approach allows for comprehensive assessment of workflows, staffing practices, device selection, training, and compliance with standard precautions. Team members may include nursing leadership, frontline staff, occupational health, infection prevention, materials management, and safety officers. This collaboration supports root cause analysis to identify contributing factors—such as improper technique, workflow inefficiencies, inadequate training, or suboptimal safety-engineered devices—and to implement targeted interventions.
Option A is inappropriate because delaying action increases risk to healthcare personnel. Option B may be part of the evaluation but is too narrow and should not occur in isolation. Option D is insufficient because discussing trends alone does not result in immediate corrective action.
The Study Guide highlights that timely, interdisciplinary performance improvement efforts are essential to reduce occupational exposures and comply with regulatory and safety standards. Convening a multidisciplinary safety team enables rapid intervention, staff engagement, and sustainable injury reduction—making option C the best answer and a high-yield CIC® exam concept.
==========
A patient with meningococcal meningitis experiences cardiac arrest. A nurse administers mouth-to-mouth breathing during CPR. Which of the following actions should the nurse take immediately?
Use oral chlorhexidine rinse
Quarantine from others for 5 days
Begin chemoprophylaxis within 24 hours
Monitor self and seek care if symptoms develop
The CBIC Certified Infection Control Exam Study Guide (6th edition) identifies Neisseria meningitidis as a highly transmissible organism spread through respiratory droplets and direct contact with oral secretions. Healthcare personnel who have unprotected, close exposure—such as mouth-to-mouth resuscitation—to a patient with meningococcal meningitis are considered high-risk contacts.
In this scenario, the nurse had direct exposure to respiratory secretions during CPR, which constitutes a significant risk for transmission. The Study Guide emphasizes that postexposure chemoprophylaxis is indicated as soon as possible, ideally within 24 hours of exposure, to prevent invasive meningococcal disease. Recommended prophylactic agents include rifampin, ciprofloxacin, or ceftriaxone, depending on contraindications and institutional protocols.
Option A is incorrect because chlorhexidine oral rinse does not eliminate systemic infection risk. Option B is inappropriate because quarantine is not required for exposed healthcare workers who receive appropriate prophylaxis. Option D is insufficient, as monitoring alone does not adequately reduce the risk of developing disease following high-risk exposure.
Rapid initiation of chemoprophylaxis is a critical infection prevention intervention and a high-yield CIC® exam concept. Early action protects the exposed healthcare worker and prevents secondary transmission within the healthcare setting.
Which of the following individuals should be excluded from receiving live attenuated influenza virus?
Pregnant persons
Healthy persons aged 2 to 49
Persons with allergies to chicken feathers
Persons simultaneously receiving an inactivated vaccine
The correct answer is A, "Pregnant persons," as they should be excluded from receiving the live attenuated influenza virus (LAIV) vaccine. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, which align with recommendations from the Centers for Disease Control and Prevention (CDC) and the Advisory Committee on Immunization Practices (ACIP), the LAIV, commonly known as the nasal spray flu vaccine, contains a live attenuated form of the influenza virus. This vaccine is contraindicated in pregnant individuals due to the theoretical risk of the attenuated virus replicating and potentially harming the fetus, despite limited evidence of adverse outcomes (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.2 - Implement measures to prevent transmission of infectious agents). Pregnant persons are instead recommended to receive the inactivated influenza vaccine (IIV), which is considered safe during pregnancy.
Option B (healthy persons aged 2 to 49) is incorrect because this group is generally eligible to receive LAIV, provided they have no other contraindications, as the vaccine is approved for healthy, non-pregnant individuals in this age range (CDC Immunization Schedules, 2024). Option C (persons with allergies to chicken feathers) is not a contraindication for LAIV; the vaccine is produced in eggs, and while egg allergy was historically a concern, current guidelines indicate that LAIV can be administered to persons with egg allergies if they can tolerate egg in their diet, with precautions managed by healthcare providers. Option D (persons simultaneously receiving an inactivated vaccine) is also incorrect, as LAIV can be co-administered with inactivated vaccines without issue, according to ACIP recommendations, as there is no significant interference between the two vaccine types.
The exclusion of pregnant persons reflects CBIC’s emphasis on tailoring infection prevention strategies, including vaccination programs, to protect vulnerable populations while minimizing risks (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.1 - Collaborate with organizational leaders). This decision is based on precautionary principles outlined in CDC and ACIP guidelines to ensure maternal and fetal safety (CDC Prevention and Control of Seasonal Influenza with Vaccines, 2023).
An infection preventionist (IP) is tasked with identifying if the Intensive Care Unit’s (ICU) central line–associated bloodstream infection (CLABSI) prevention practices are consistent with current best practices. Which of the following quality improvement tools should the IP construct?
Gap analysis
Root cause analysis
Failure mode and effect analysis (FMEA)
Strengths, weaknesses, opportunities, and threats (SWOT) analysis
The Certification Study Guide (6th edition) clearly distinguishes among quality improvement tools based on their purpose and timing. When the goal is to determine whether current practices align with evidence-based standards or best practices, the most appropriate tool is a gap analysis. A gap analysis systematically compares current state practices—such as ICU CLABSI prevention policies, procedures, and compliance data—with the desired state, which is defined by nationally recognized guidelines and best practices.
The study guide emphasizes that gap analysis is particularly useful for program evaluation, policy review, and baseline assessment before implementing improvements. In this scenario, the IP is not responding to an adverse event, nor is the IP proactively predicting failures, but rather assessing alignment with best practices, which is the core function of a gap analysis.
The other tools serve different purposes. Root cause analysis (RCA) is used after an adverse event (such as a CLABSI) to identify contributing factors. Failure mode and effect analysis (FMEA) is a prospective risk assessment tool used to anticipate where processes might fail. SWOT analysis is a strategic planning tool and is not sufficiently specific for evaluating compliance with infection prevention standards.
Because CIC exam questions frequently test the ability to select the right tool for the right situation, recognizing gap analysis as the appropriate choice in this context is essential.
An infection preventionist is calculating measures of central tendency regarding duration of a surgical procedure using this data set: 2, 2, 3, 4, and 9. Which of the following statements is correct?
The median is 2.
The mode is 3.
The mean is 4.
The standard deviation is 7.
Measures of central tendency (mean, median, mode) and dispersion (standard deviation) are statistical tools used to summarize data, such as the duration of surgical procedures, which can help infection preventionists identify trends or risks for surgical site infections. The Certification Board of Infection Control and Epidemiology (CBIC) supports the use of data analysis in the "Surveillance and Epidemiologic Investigation" domain, aligning with epidemiological principles outlined by the Centers for Disease Control and Prevention (CDC). The question provides a data set of 2, 2, 3, 4, and 9, and requires determining the correct statement by calculating these measures.
Mean: The mean is the average of the data set, calculated by summing all values and dividing by the number of observations. For the data set 2, 2, 3, 4, and 9:(2 + 2 + 3 + 4 + 9) ÷ 5 = 20 ÷ 5 = 4. Thus, the mean is 4, making Option C correct.
Median: The median is the middle value when the data set is ordered. With five values (2, 2, 3, 4, 9), the middle value is the third number, which is 3. Option A states the median is 2, which is incorrect.
Mode: The mode is the most frequently occurring value. In this data set, 2 appears twice, while 3, 4, and 9 appear once each, making 2 the mode. Option B states the mode is 3, which is incorrect.
Standard Deviation: The standard deviation measures the spread of data around the mean. For a small data set like this, the calculation involves finding the variance (average of squared differences from the mean) and taking the square root. The mean is 4, so the deviations are: (2-4)² = 4, (2-4)² = 4, (3-4)² = 1, (4-4)² = 0, (9-4)² = 25. The sum of squared deviations is 4 + 4 + 1 + 0 + 25 = 34. The variance is 34 ÷ 5 = 6.8, and the standard deviation is √6.8 ≈ 2.61 (not 7). Option D states the standard deviation is 7, which is incorrect without further context (e.g., a population standard deviation with n-1 denominator would be √34 ≈ 5.83, still not 7).
The CBIC Practice Analysis (2022) and CDC guidelines encourage accurate statistical analysis to inform infection control decisions, such as assessing surgical duration as a risk factor for infections. Based on the calculations, the mean of 4 is the only correct statement among the options, confirming Option C as the answer. Note that the standard deviation of 7 might reflect a miscalculation or misinterpretation (e.g., using a different formula or data set), but with the given data, it does not hold.
Which of the following processes is essential for endoscope reprocessing?
Intermediate level disinfection and contact time
Pre-cleaning, leak testing, and manual cleaning
Inspection using a borescope and horizontal storage
Leak testing, manual cleaning, and low level disinfection
The correct answer is B, "Pre-cleaning, leak testing, and manual cleaning," as these processes are essential for endoscope reprocessing. According to the Certification Board of Infection Control and Epidemiology (CBIC) guidelines, proper reprocessing of endoscopes is critical to prevent healthcare-associated infections (HAIs), given their complex design and susceptibility to microbial contamination. The initial steps of pre-cleaning (removing gross debris at the point of use), leak testing (ensuring the endoscope’s integrity to prevent fluid ingress), and manual cleaning (using enzymatic detergents to remove organic material) are foundational to the reprocessing cycle. These steps prepare the endoscope for high-level disinfection or sterilization by reducing bioburden and preventing damage, as outlined in standards such as AAMI ST91 (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.3 - Ensure safe reprocessing of medical equipment). Failure at this stage can compromise subsequent disinfection, making it a non-negotiable component of the process.
Option A (intermediate level disinfection and contact time) is an important step but insufficient alone, as intermediate-level disinfection does not achieve the high-level disinfection required for semi-critical devices like endoscopes, which must eliminate all microorganisms except high levels of bacterial spores. Option C (inspection using a borescope and horizontal storage) includes valuable quality control (inspection) and storage practices, but these occur later in the process and are not essential initial steps; vertical storage is often preferred to prevent damage. Option D (leak testing, manual cleaning, and low level disinfection) includes two essential steps (leak testing and manual cleaning) but is inadequate because low-level disinfection does not meet the standard for endoscopes, which require high-level disinfection or sterilization.
The emphasis on pre-cleaning, leak testing, and manual cleaning aligns with CBIC’s focus on adhering to evidence-based reprocessing protocols to ensure patient safety and prevent HAIs (CBIC Practice Analysis, 2022, Domain III: Infection Prevention and Control, Competency 3.4 - Implement environmental cleaning and disinfection protocols). These steps are mandated by guidelines to mitigate risks associated with endoscope use in healthcare settings.
A construction project is completed at a healthcare facility and the construction barriers will be removed. Prior to using the space for patient care, an infection preventionist should recommend:
Sampling for airborne contaminants after construction.
Stocking supply rooms as soon as the rooms are available.
Testing the water for Legionella and other waterborne pathogens.
Inspecting and cleaning ducts if needed and balancing the ventilation system.
The Certification Study Guide (6th edition) emphasizes that restoration of a safe environment of care following construction or renovation is essential before patient occupancy. A primary concern after construction is the potential contamination and disruption of the heating, ventilation, and air conditioning (HVAC) system, which plays a critical role in infection prevention by controlling airflow, pressure relationships, and filtration.
Inspecting and cleaning air ducts as needed—and ensuring that the ventilation system is properly balanced—helps confirm that airflow is functioning as designed, including appropriate air exchanges, pressure differentials, and filtration efficiency. The study guide highlights that construction activities can introduce dust, debris, and microorganisms (including fungal spores) into ductwork, which may subsequently be disseminated into patient care areas if not addressed. Proper HVAC verification is a key component of post-construction clearance following an Infection Control Risk Assessment (ICRA).
The other options are not recommended as routine first steps. Air sampling is not advised because results are difficult to interpret and do not reliably predict infection risk. Stocking supplies before environmental clearance risks contamination of clean items. Routine water testing is not required unless water system disruption or stagnation occurred and is guided by a facility’s water management program rather than construction completion alone.
CIC exam questions frequently test post-construction readiness activities, reinforcing that HVAC inspection, cleaning, and balancing are critical prerequisites for safely reopening patient care spaces.
Copyright © 2021-2026 CertsTopics. All Rights Reserved

